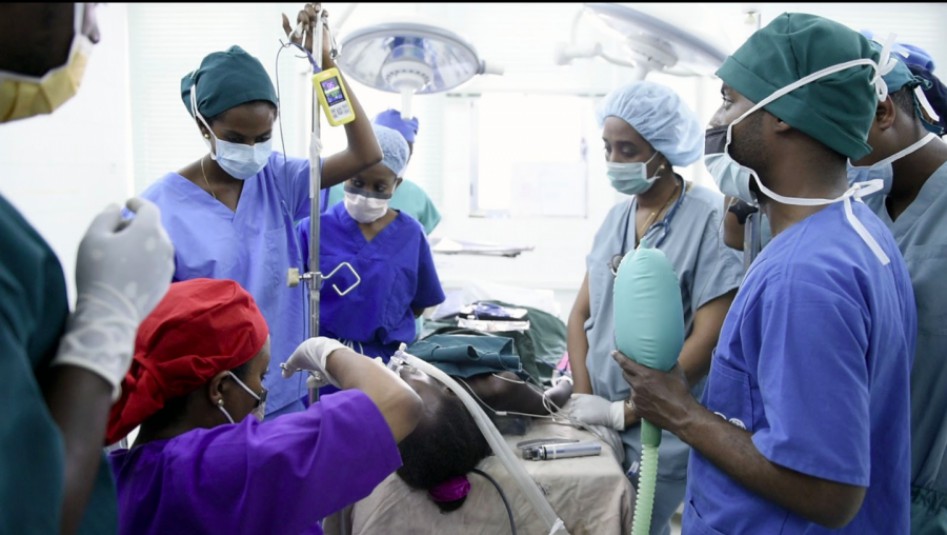
Surgical Teamwork
Strengthening multidisciplinary teamwork within and beyond the operating room

Lifebox makes surgery and anesthesia safer through tools, training, and partnerships.
In parts of the world, the risk of death following surgery can be 22 times higher than in a high-income country.¹
Lifebox addresses critical gaps in surgical safety through tools, training, and partnerships. We focus on three core pillars of safer surgery – improving anesthesia safety, reducing surgical infection, and strengthening surgical teamwork. So far, this approach has made surgery safer for 181 million patients around the world.
All of this work is rooted in the WHO Surgical Safety Checklist – a simple communication tool that has been proven to reduce complications and deaths from unsafe surgery by up to 40%.
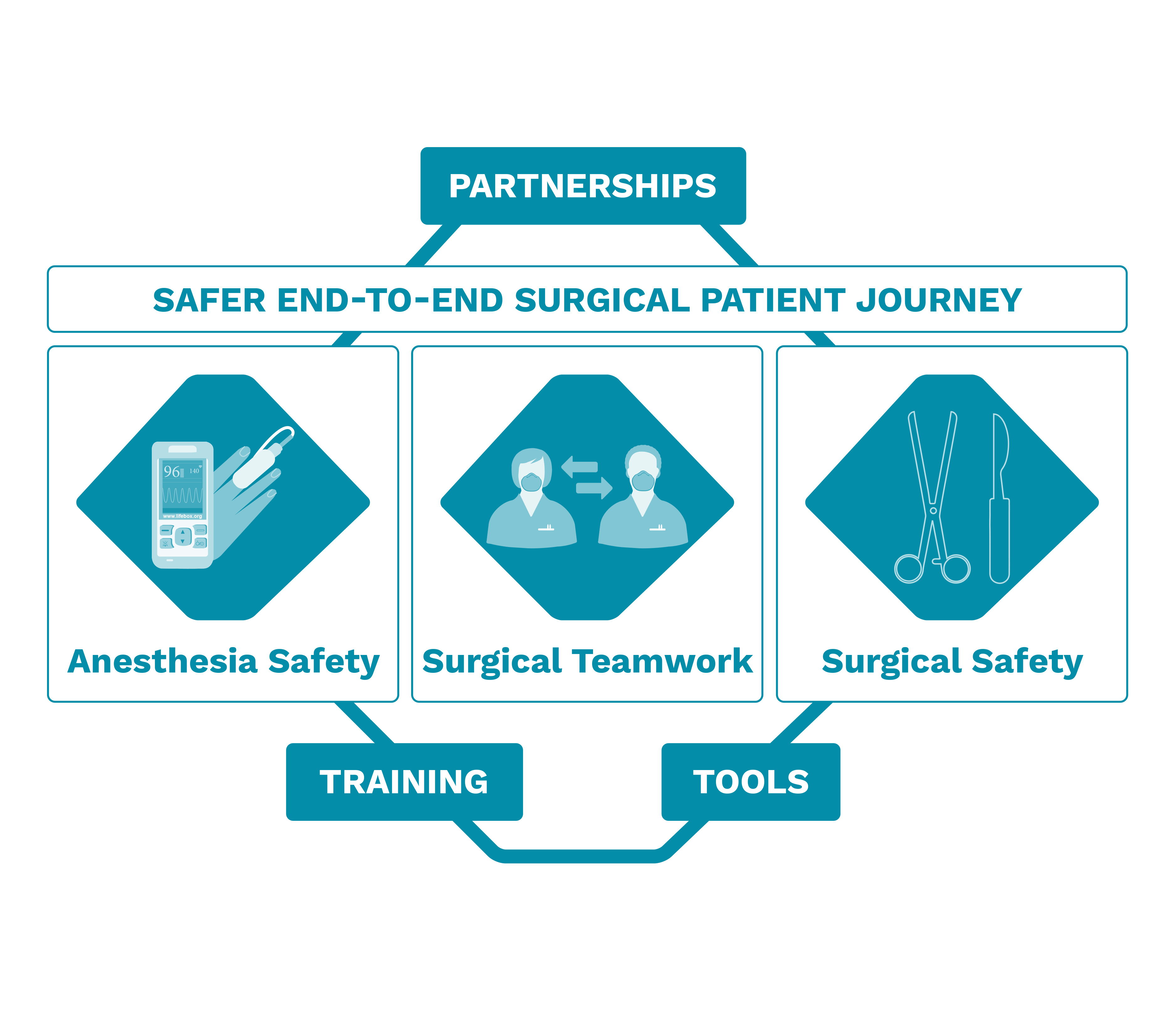
Working across three pillars of safer surgery, Lifebox makes surgery and anesthesia safer for every patient, every time through tools, training, and partnerships.

Strengthening multidisciplinary teamwork within and beyond the operating room
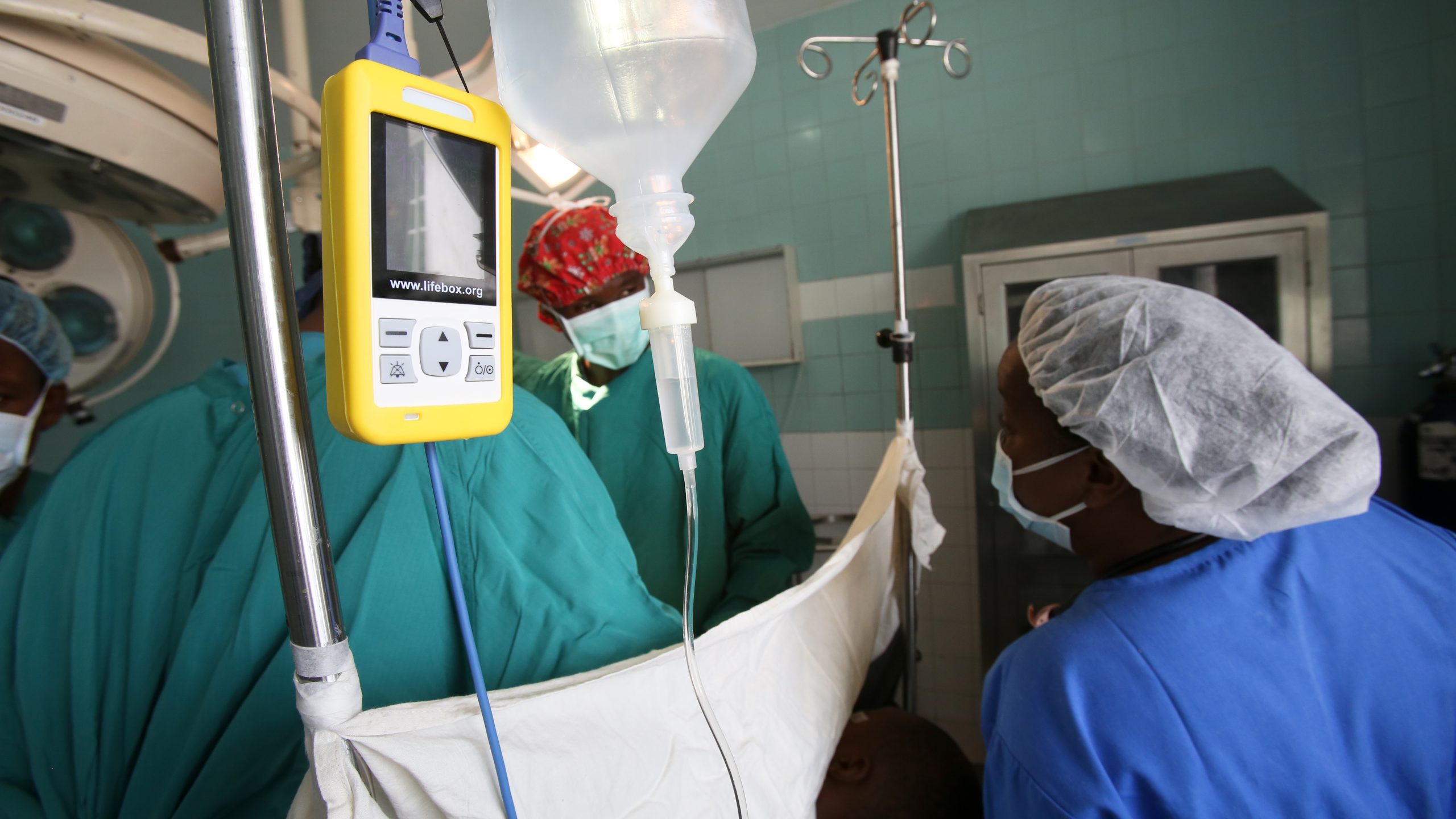
Making anesthesia safer through improved patient monitoring
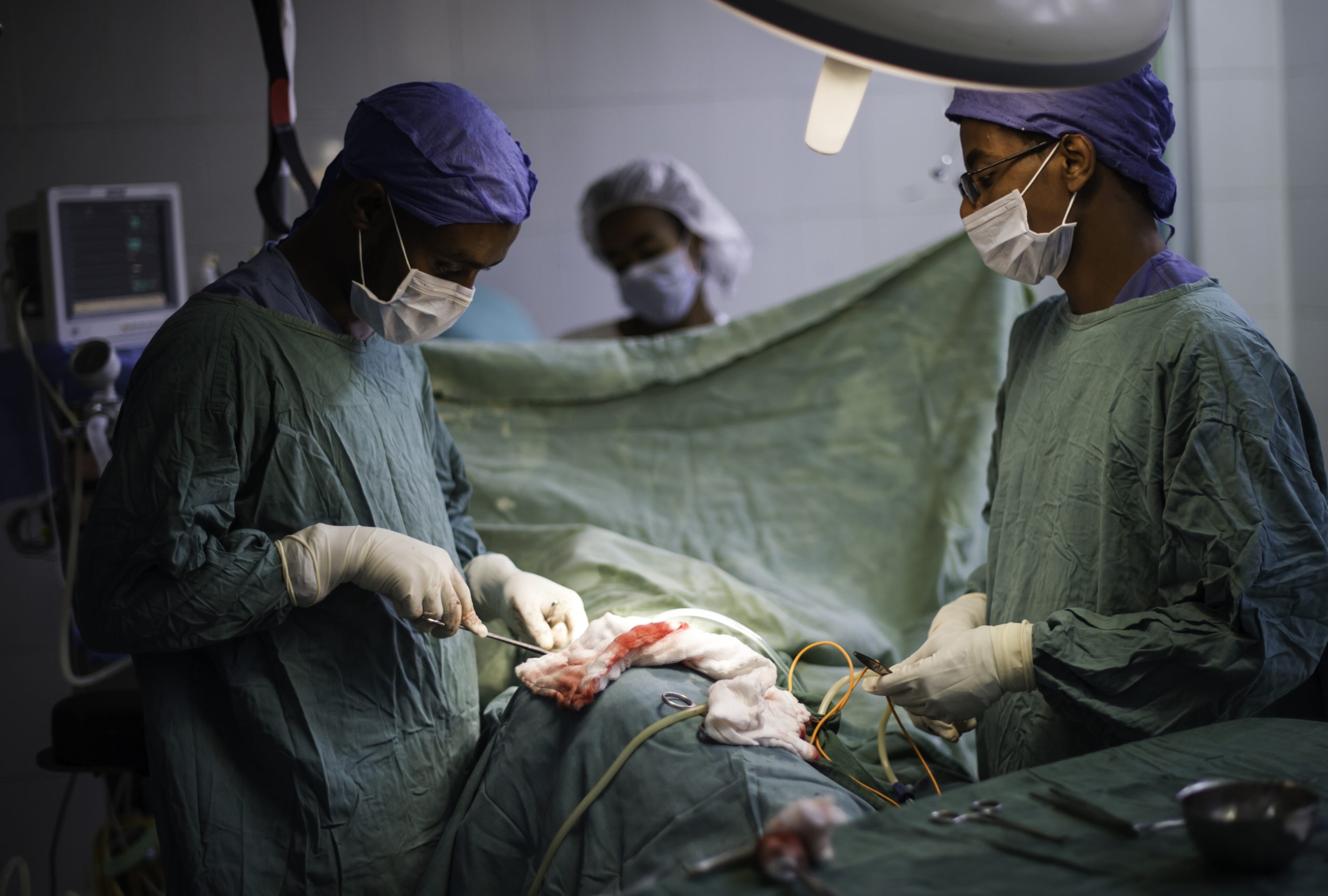
Clean Cut®: our surgical quality improvement program

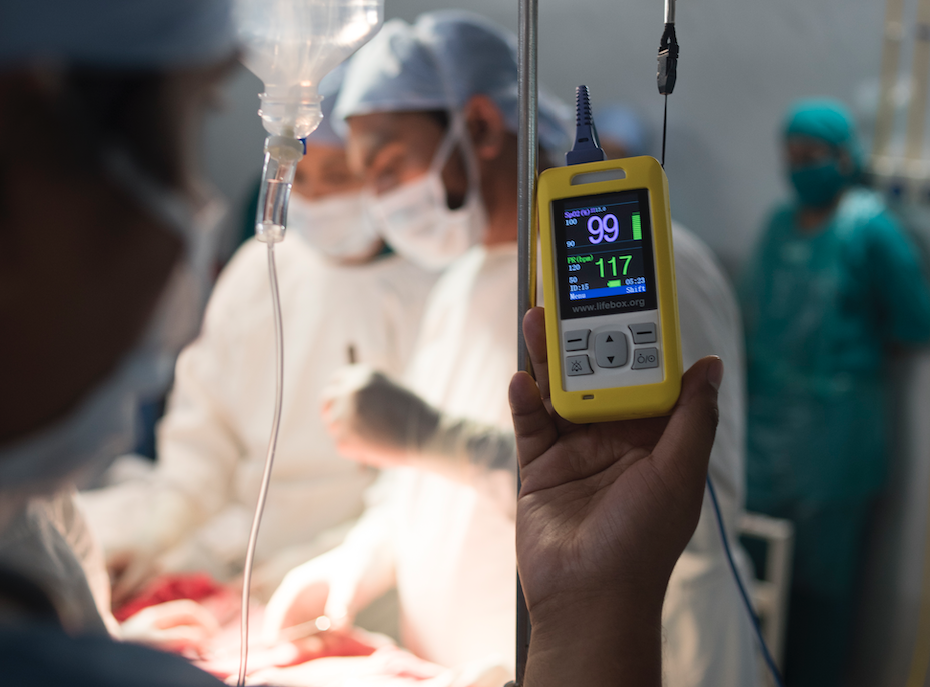
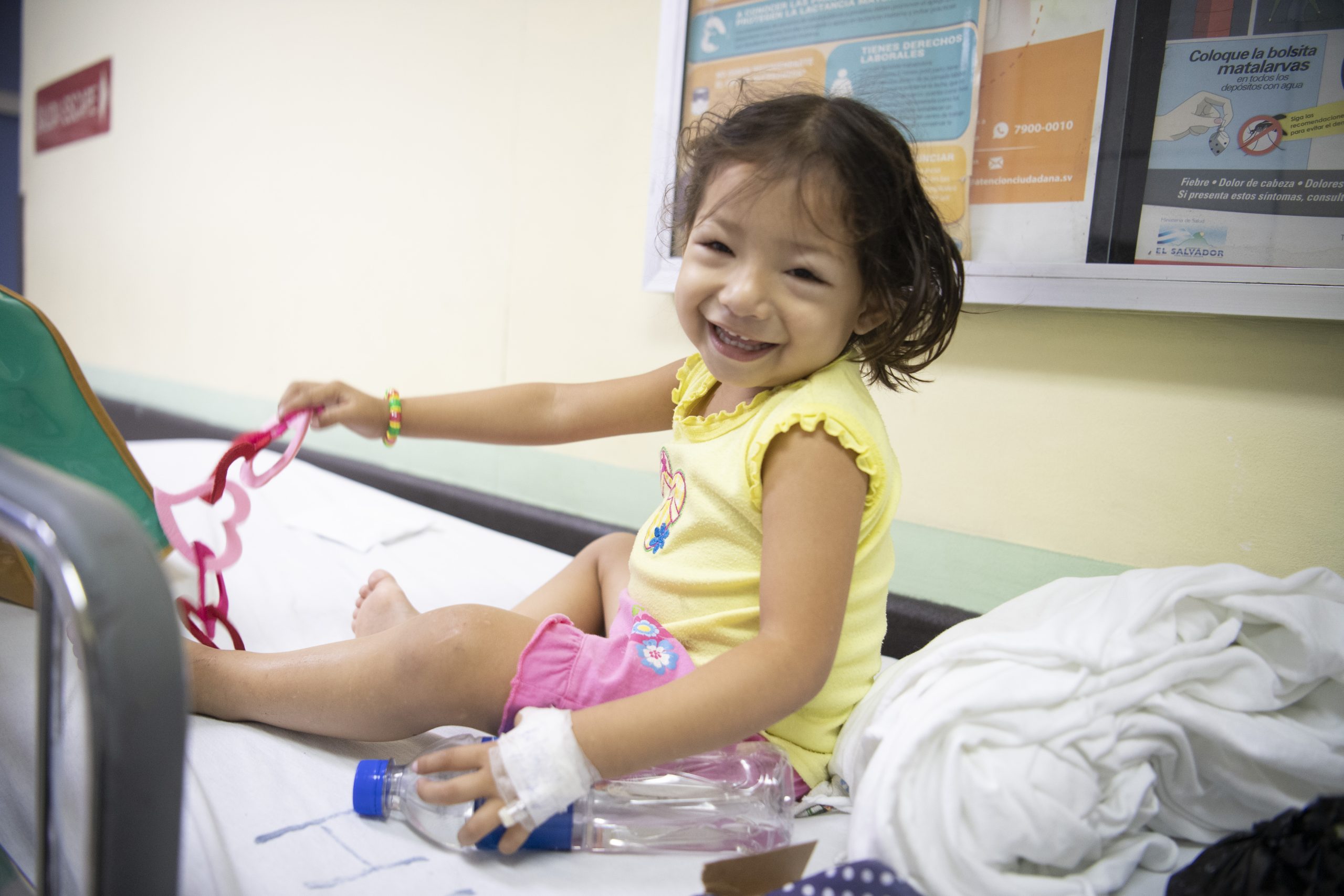
Our work relies on the generosity of our donors. Help equip healthcare providers around the world with essential tools and training to make surgery safer. Please make a donation today and fund Lifebox' work.
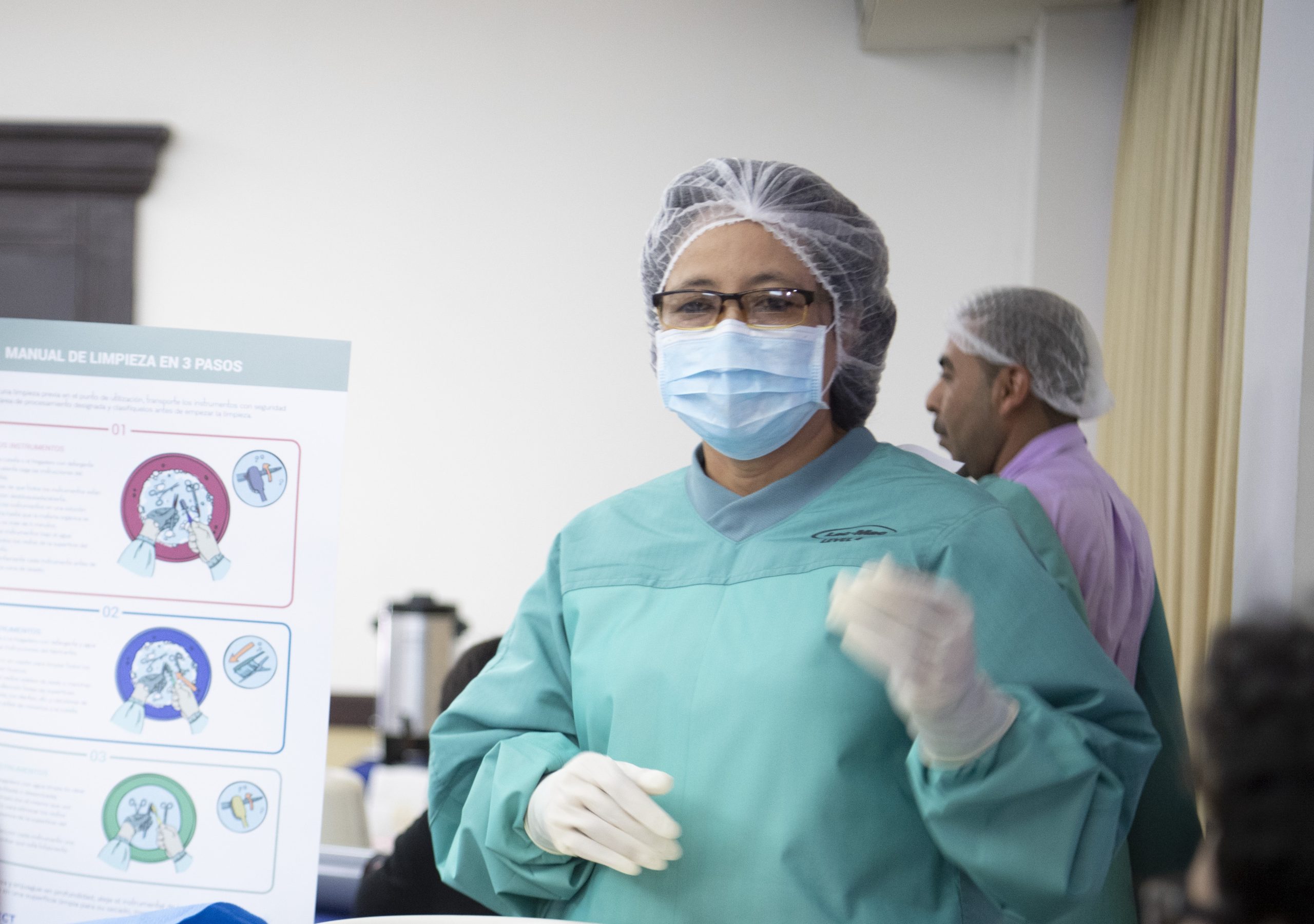
Our open access online learning platform

Updates from across the world on our safer surgery work
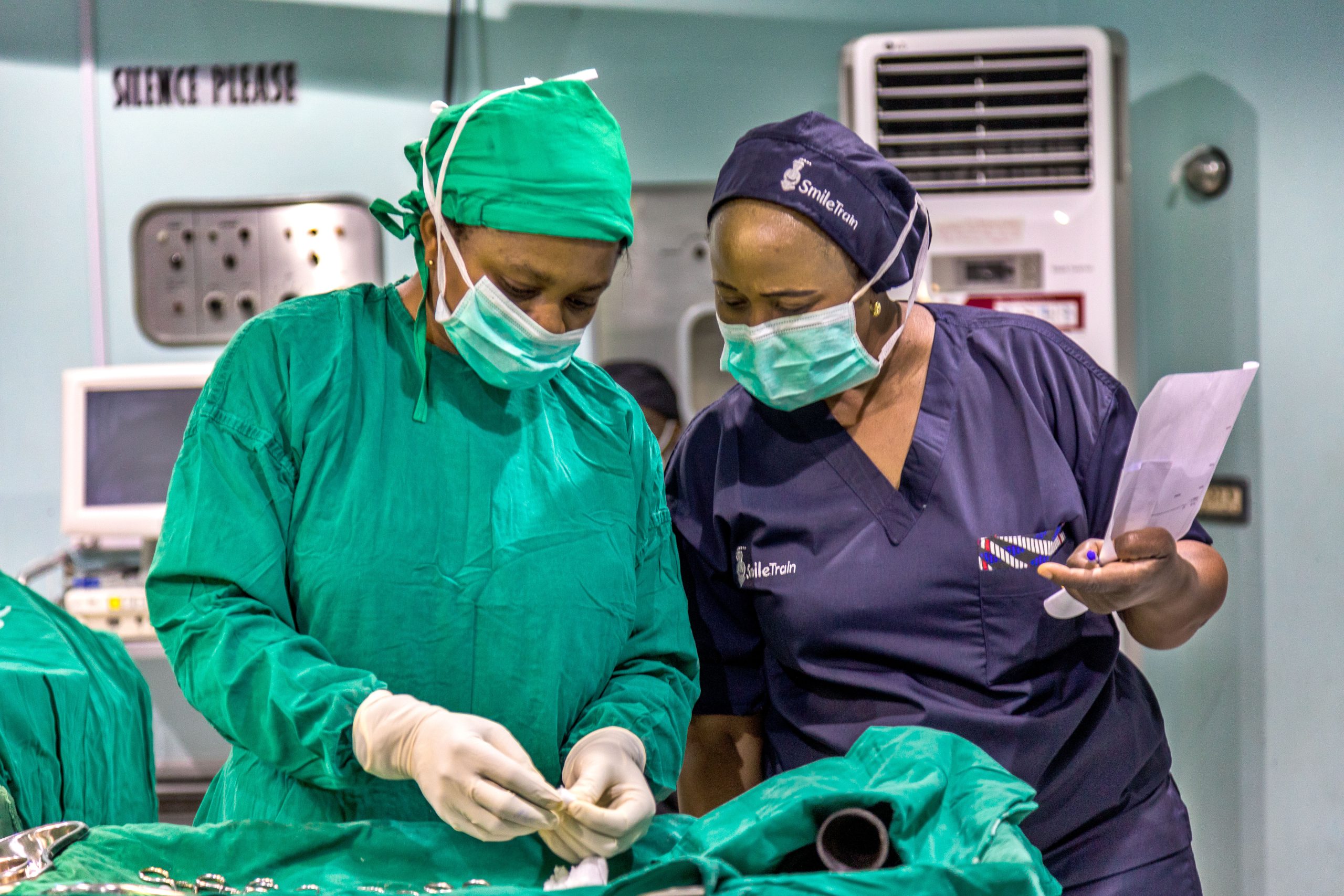
Elevating the quality and safety of cleft and pediatric surgery
¹ Uribe-Leitz T, Jaramillo J, Maurer L, et al. Variability in mortality following caesarean delivery, appendectomy, and groin hernia repair in low-income and middle-income countries: a systematic review and analysis of published data. Vol. 4, The Lancet Global Health; 2016. p e165-e174, https://doi.org/10.1016/S2214-109X(15)00320-4