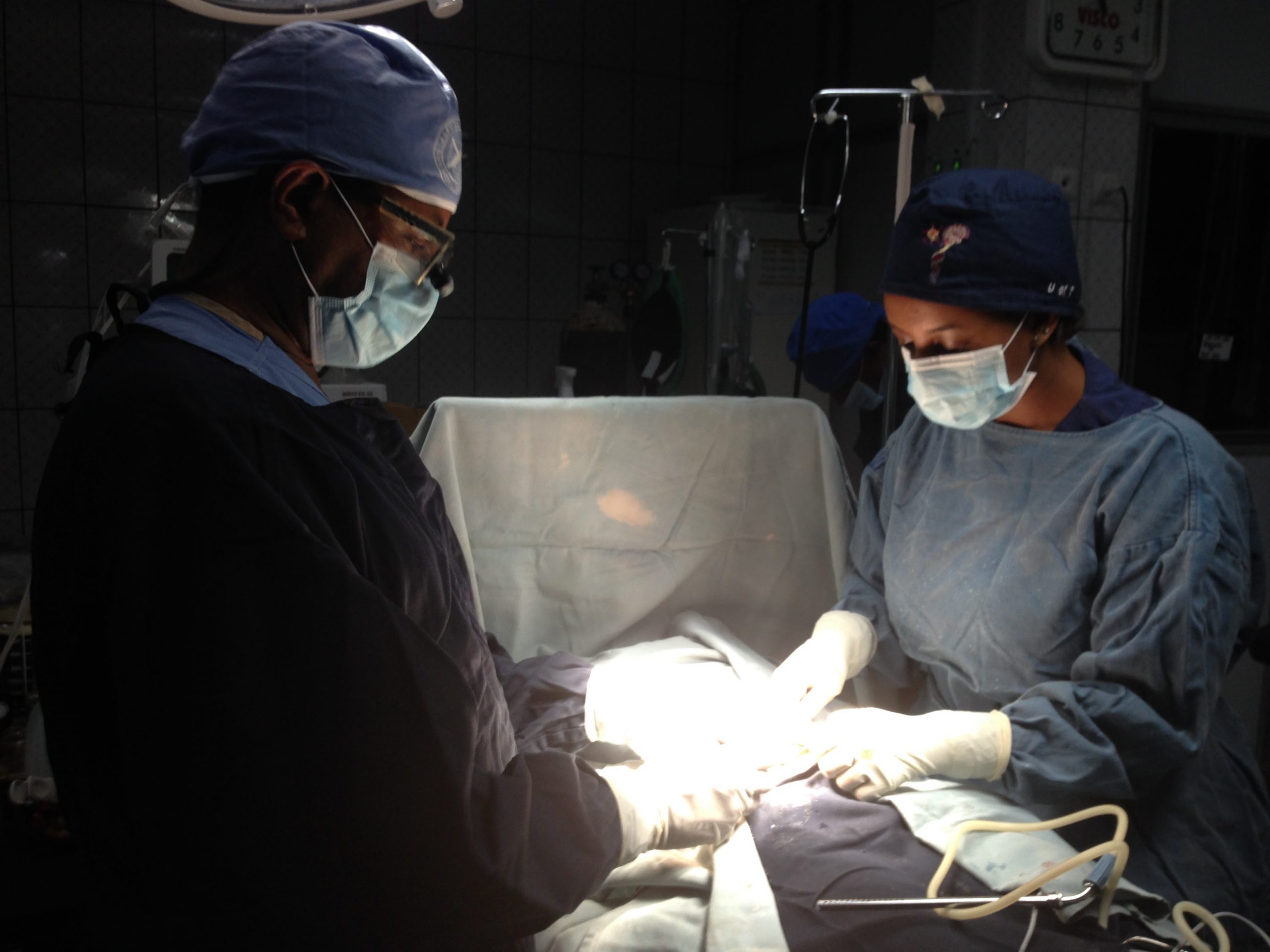
A Growing Challenge, a Growing Commitment
Professor Miliard Derbew talks to Lifebox on the challenges of providing safe surgical pediatric care and safe surgery in East Africa
“We need safe surgery to be practiced for good outcomes. We need to scale training and capacity building. We need research and innovation in pediatric surgical care.” Professor Miliard Derbew

Lifebox Board Member, Professor Miliard Derbew, is a pediatric surgeon from Ethiopia. He serves as CEO of King Faisal Hospital, Kigali – Rwanda’s largest referral hospital – and Professor of Pediatric Surgery at the College of Health Sciences, Addis Ababa University. This interview is part of the Smile Train-Lifebox Safe Surgery and Anesthesia Initiative content series.
“I have been practicing pediatric surgery in Eastern Africa for 24 years, mainly in Ethiopia. My passion has always been working with kids, and when I was a student, my aim was to become a pediatrician. When I graduated, I found the surgery rotation very interesting, and having the opportunity to do pediatric surgery united my love of helping kids and surgery. This was the best contribution I could make to my community and my country. It’s a hard specialization that needs a lot of commitment. You have to live for your profession!

Professor Miliard Derbew, Professor of Pediatric Surgery and Lifebox Board Member
It is particularly challenging to work as a pediatric surgeon in the region where I practice due to limited resources. In pediatric surgery, human resources are among both the most important and the most limited.
Governments and policymakers do not give the necessary attention to support pediatric training programs. They think any surgeon can provide pediatric surgery. Of course, they can do it, but it’s the outcome of the surgery that is important. Operating on a child is not the same as operating on a small adult. It’s completely different. Children need their own surgeons, anesthesiologists, pediatricians, nurses, and NICU nurses. They need expert management. It’s the most challenging environment, and with children making up so much of the population in Eastern Africa, we need pediatric surgeons.
Three years ago, I evaluated 12 countries in the Eastern, Central and Southern African regions. There were less than 50 pediatric surgeons for a population close to half a billion, with children making up half of that. In Rwanda, where I am based now, there is one pediatric surgeon in the country. South Sudan and Namibia have no pediatric surgeons. Although we are increasing the number of pediatric surgeons, the pediatric population is also growing.
In Ethiopia, more than 50% of the population is below the age of 15. For many years, I was one of the only two pediatric surgeons in Ethiopia. In 2010, the Tikur Anbessa Hospital, School of Medicine at Addis Ababa University, and the Government of Ethiopia wanted to expand the pediatric surgical program. We partnered with the University of Toronto and Vellore Christian Medical School in India and started a fellowship program in pediatric surgery. We now have 17 pediatric surgeons practicing in Ethiopia, and nine more will join us soon having passed the COSECSA, FCS program. This is a great achievement, and we hope it will help to mitigate the surgical burden that we face.
Despite these efforts, the neonatal mortality rate for surgical patients is still high. We are not in the position to save lives, because we lack the technology and the support facilities. To save lives, you need the whole system, such as a well-established neonatal intensive care unit (NICU), supports like parenteral nutrition (intravenous feeding for neonates), and experienced NICU nurses.
With a high fertility rate, we also have high numbers of children born with congenital conditions. These treatments are often challenging. One of the most common challenges we see in my institution happens when babies are born with tracheoesophageal fistulas, where the esophagus and the trachea are connected. Usually, we only see this child three or four days after birth. During this time, they will have had no hydration or nourishment, meaning they arrive malnourished and dehydrated. Many already have an infection, usually a lung infection. These children are clearly a surgical and anesthesia risk. We can do the surgery, but the child’s esophagus is not ready for feeding for seven to ten days after the operation, which means another week with no food for this child.
In a high-income country (HIC), this child would have proper parenteral nutrition to build up their strength before and after surgery. In low- and middle-income countries (LMICs), we do not have this, and so we have high mortality rates in cases like this. It’s always heartbreaking. The surgery takes between two and four hours, and as you make all of these efforts to save the child, you know the outcome will likely not be good.
Malnutrition is also common and life-threatening among patients with cleft lip and/or palate. In order to reach a healthy weight for surgery, they often need nutritional support. Their mothers need guidance on how to feed them effectively. They then need not only specialized pediatric surgery, but also a team of providers working with the surgical team to provide integrated, essential cleft care.
We cannot have good surgical outcomes without the full system, including infrastructure and human resources, because all of these things need to be in place to make true change in neonatal surgery. This is the main problem that we face. Children in LMICs are not getting the necessary attention from policymakers and governments.
The burden of surgical conditions is only increasing. We need safe surgery to be practiced for good outcomes. We need to scale training and capacity building. We need research and innovation in pediatric surgical care.
This is where Lifebox and Smile Train come in with the Smile Train-Lifebox Safe Surgery and Anesthesia Initiative. These are two organizations that have been working within the surgical ecosystem: Lifebox with a focus on safe surgery and anesthesia, and Smile Train with a focus on the treatment of cleft lip and palate. Through this Initiative, these two organizations will strengthen the capacity of surgical teams around the world, bringing a much-needed focus on cleft lip and palate surgery and pediatric surgery more broadly. This will improve pediatric surgical and anesthesia care for thousands of children globally.
While partnerships like this build critical capacity, pediatric surgery also needs the attention and investment of policymakers. Since 2015, many countries have drastically reduced their infant and pediatric mortality rates through vaccinations and nutrition.
If we want to reduce infant mortality further, we need interventions to work deeply on the surgical management of children.
However, as I have worked as a pediatric surgeon for more than 20 years, I have also seen change and progress firsthand. I now see students who were once my patients. My patients have gone on to become nurses and medical students, and one has already become a doctor! They remember me and that I operated on them! This makes me very happy. Even though there are many heartbreaking moments, there are also wonderful experiences in this field.”
Find out more about the Smile Train-Lifebox Safe Surgery and Anesthesia Initiative here.

