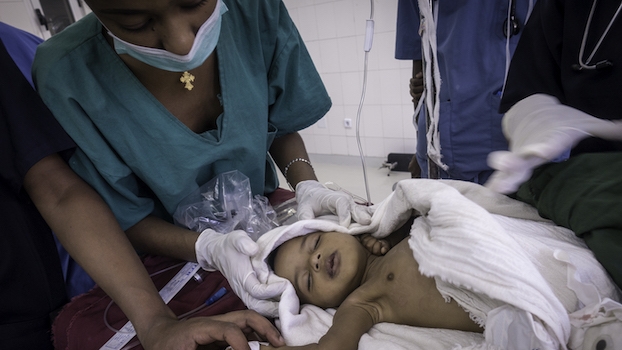
Lifebox is dedicated to improving the safety of surgery and anesthesia around the world through training, tools, and partnerships. Lifebox has opportunities for Fellows to work on programs to reduce surgical infection, increase access to pulse oximetry for safe anesthesia, and improve surgical teamwork.
Lifebox is offering a variety of fellowship opportunities to clinical, research, and pedagogic professionals at all stages of their careers. Fellows are assigned a mentor and work directly with Lifebox team members and partners to achieve programmatic and/or research objectives. Lifebox Fellows gain first-hand experience in program delivery, training, and research, with the objective of improving the safety of surgical and anesthesia care in resource-limited settings.
Each Fellow works with their mentor to define individual goals and is encouraged to propose ideas for program implementation, research, or methodologies for measuring impact. Recent Lifebox Fellows have developed training materials, implemented quality improvement programs, and analyzed evaluation data. The majority have presented original research at professional conferences and published on their work with Lifebox.
We are look for a minimum six month, ideally one year, commitment with a flexible time commitment from four days per month to full-time depending on the position, interests, and availability of candidates. We are able to offer an honorarium of US$10,000 to those able to commit 60% of their time; this will be prorated based on the agreed time commitment.
If you are interested in becoming a Lifebox Fellow, please send us an email to [email protected] outlining your interests and providing your CV.
Additional details on the Lifebox Safe Surgery Fellows program:
The Fellows will develop and deliver research and quality improvement initiatives to enhance the safety of surgery and anesthesia in low and middle income countries (LMICs). Fellows will work in close collaboration with hospitals, clinicians, governmental bodies, and other stakeholders. We particularly encourage candidates from the Global South to apply.
The objectives of the Fellows Program are to:
1. Contribute to measurable improvement in the safety of surgery and anesthesia in a low-resource setting;
2. Work with local clinicians, health ministries, fellow residents and trainees, and multi-disciplinary teams to develop and implement locally-initiated, adapted, and effective surgical quality improvement initiatives;
3. Undertake rigorous original research to drive and advocate for safer surgery and anesthesia locally and globally;
4. Develop skills and expertise as future leaders in the implementation of perioperative quality improvement programs.
The Fellowship offers:
– An opportunity to build skills and experience in quality improvement, training, human-centered design, operations management, and perioperative research, particularly as they pertain to challenges in LMICs;
– Strong academic mentorship from clinical leaders – a Lifebox trustee or closely affiliated faculty member – in patient safety, quality improvement, and health systems strengthening;
– Time to pursue research in perioperative improvement in line with the Fellow’s own research interests;
– The opportunity to generate impactful, publishable academic work that will improve how perioperative care is delivered;
– Exposure to program development, delivery, and implementation, aspects of international development work, impact of device distribution, human-centered design, training and education pedagogy and delivery, and the workings of a global nonprofit;
– Access and opportunity to collaborate with a robust international network of top-quality clinicians, research institutes, and other stakeholders engaged in ongoing programmatic work.