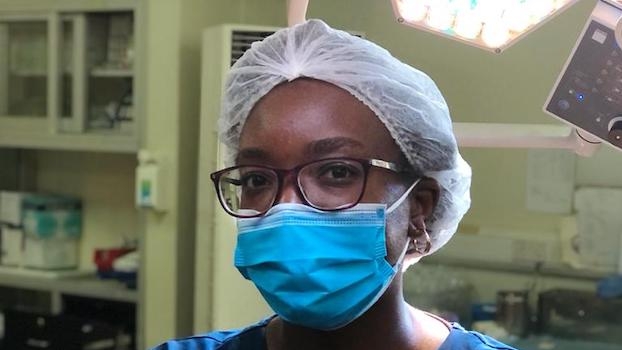
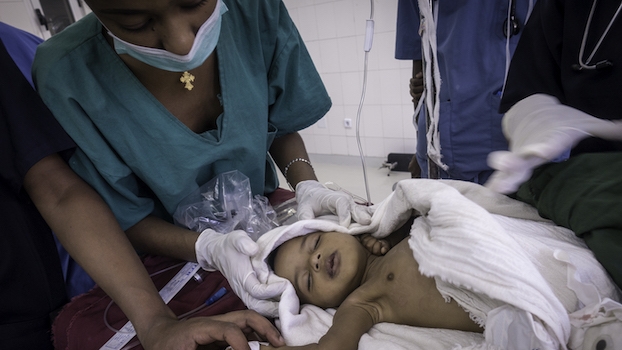
Lifebox features on the BBC
'One Crucial Piece of Equipment': Improving anesthesia monitoring with The Smile Train-Lifebox Capnograph.
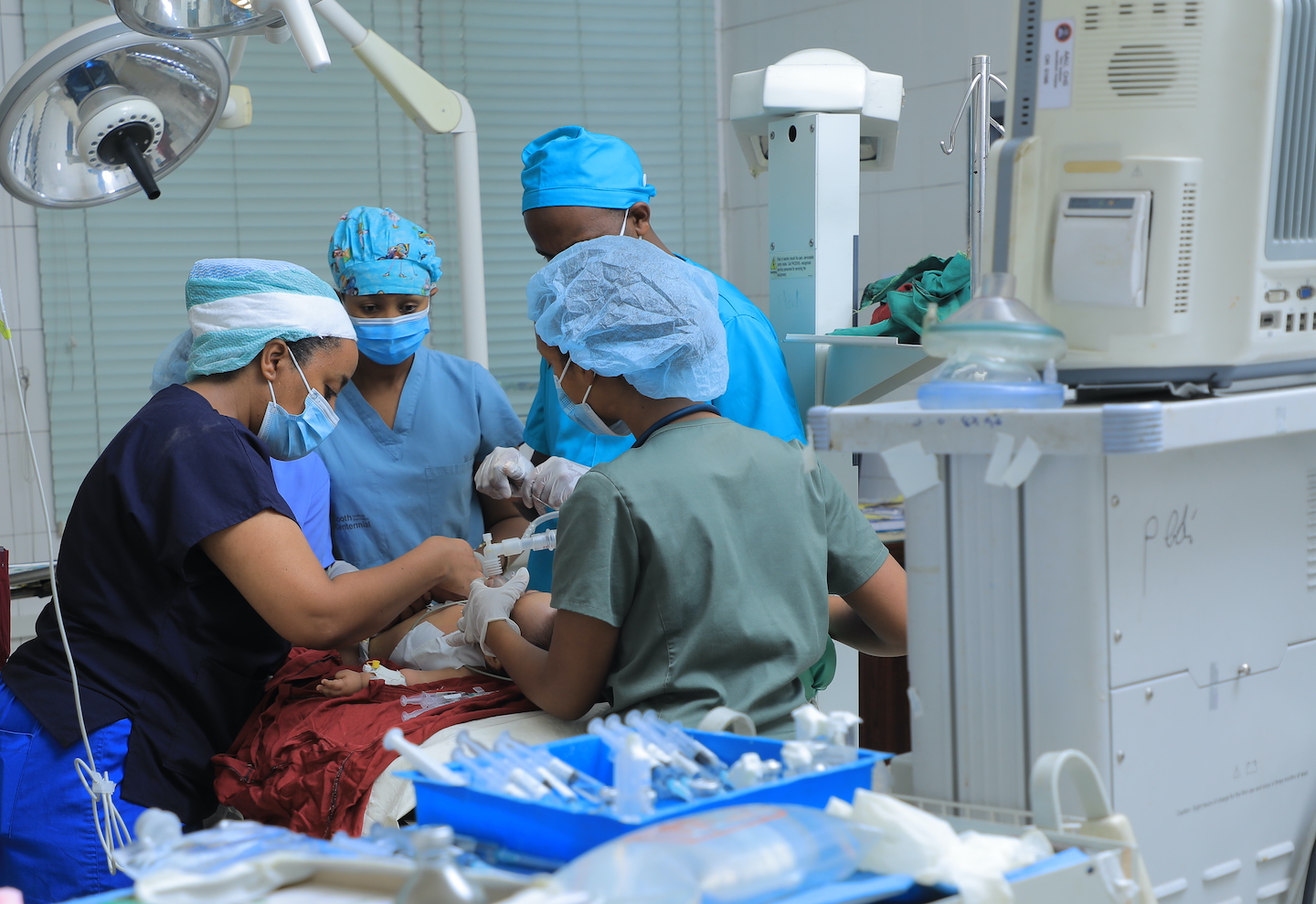
Lifebox is a global nonprofit making surgery and anesthesia safer worldwide. Through tools, training, and partnerships we make surgery safer for every patient, every time.
Introducing the Lifebox Light: A low-cost, high quality surgical headlight for low-resource setting operating rooms


'One Crucial Piece of Equipment': Improving anesthesia monitoring with The Smile Train-Lifebox Capnograph.
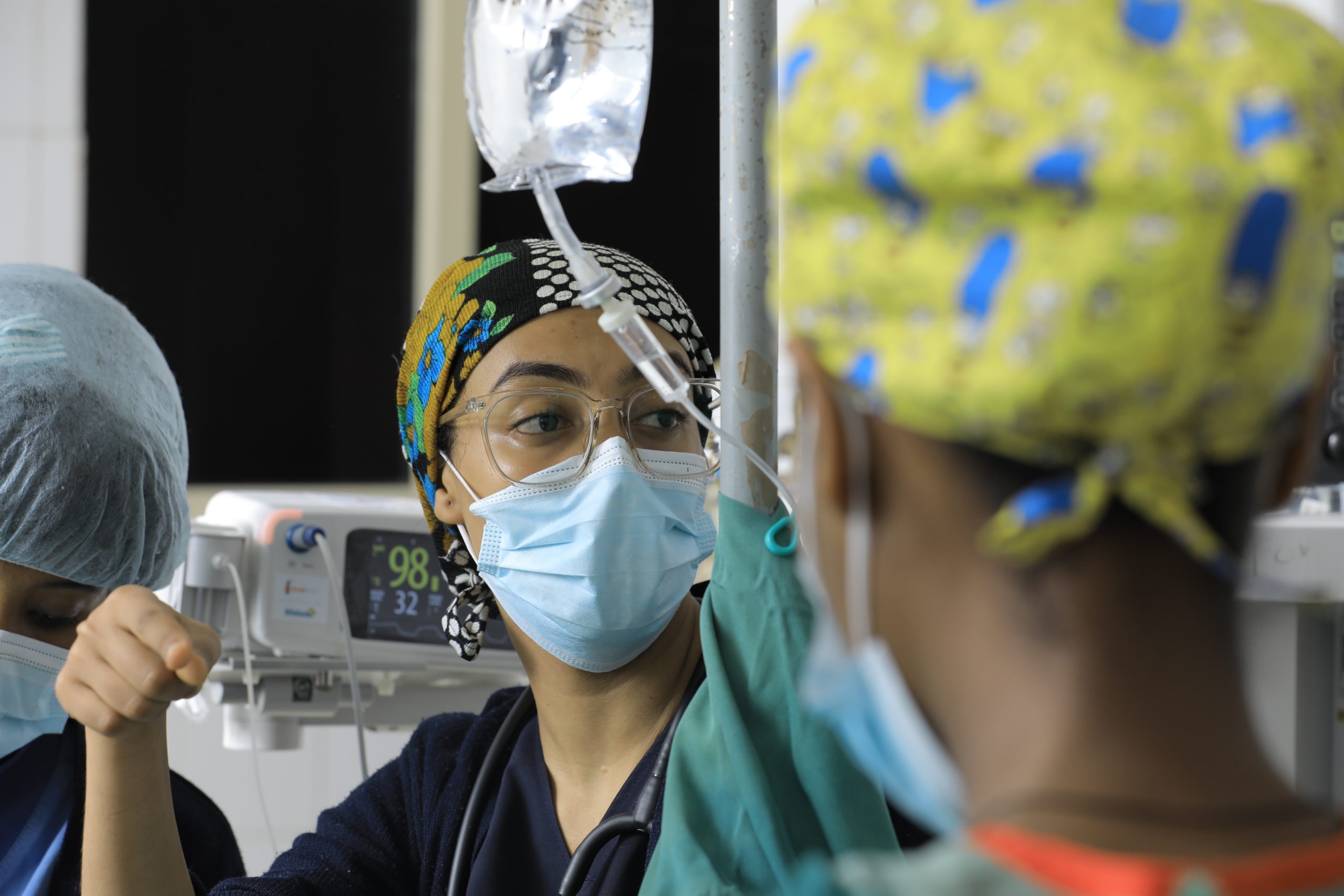
SINGAPORE- March 6, 2024 – In a significant move to improve safety for millions of people undergoing surgery each year, the world’s largest cleft-focused organization, Smile Train, and the safer surgery global nonprofit, Lifebox, have come together to urge health care systems and equipment standard guidelines, including those set by...
Making surgery safer for every patient, every time.
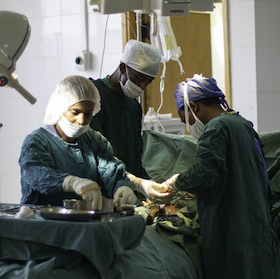
Surgeries made safer
Healthcare providers trained in safer surgery and anesthesia
Pulse oximeters distributed to frontline providers across 116 countries worldwide