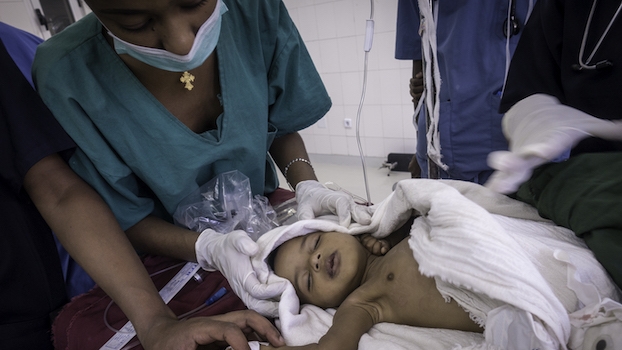
A frontline view of strengthening safer surgery in Rwanda
On this World Health Day, the call to act “Together for health. Stand with science” reminds us that better health outcomes do not come from good intentions alone. They come from using evidence, strengthening systems, and supporting health workers to provide safer care every day. In Rwanda, I have seen what that looks like in the operating theatre. Over 16 years working in surgical care, I have witnessed the risks patients face when surgery is not safe. I have often wondered how best to express this truth — whether in a book, a song, or a sentence written on every theatre wall: safe surgery saves lives.
That truth has stayed with me because I have seen how small overlooked actions can lead to devastating harm. A missed count. Poor infection prevention. Antibiotics used without clear indication. These may seem like routine details, but in surgery, they can mean infection, prolonged recovery, repeat operations, or even death. I will never forget one thoracotomy case. At the final count, a surgical ‘peanut’ was missing. We searched for three hours while the patient remained on the table with an open chest. Although it was eventually found and removed, the patient later developed a serious infection and had to return to surgery several times for washouts. For all of us involved, it was a painful reminder of how deeply patient safety depends on consistent systems and shared accountability. Experiences like this shaped my commitment to safer surgery and later motivated my involvement in Clean Cut, a surgical site infection prevention program implemented by Lifebox in selected hospitals in Rwanda. For me, the value of the program was not only in introducing tools and processes, but in helping teams reflect on everyday practice and improve the way we work together.
One of the clearest examples came from something very simple: counting gauze correctly. At one hospital, compliance with gauze counts was just 6% at the start. Through training, teamwork, and adaptation of the WHO Surgical Safety Checklist to fit local needs, that figure rose to 100% by the end of the program. It may sound like a small change, but it represented a growing accountability, better communication, and a stronger culture of safety. Clean Cut focuses on six essential practices that help reduce surgical infections: proper use of the checklist, effective skin preparation, ensuring the sterility of instruments and linens, accurate gauze counts, and appropriate antibiotic use. Every two weeks, data were collected and reviewed, and each month teams received feedback and reflected on progress. Nurses, surgeons, anesthetists, and support staff all had a role to play, and over time those small, consistent efforts began to change habits and expectations.
One of the most meaningful changes I saw was in the use of antibiotics. Before this work, it was common to give post-operative antibiotics broadly, including to many mothers after cesarean section, whether they were truly needed or not. Over time, with stronger protocols and more deliberate decision-making, that began to shift. Antibiotics were used more appropriately, helping protect patients while also supporting the broader effort to address antimicrobial resistance. For me, this was also a practical change. I remember spending long night shifts giving antibiotics routinely to post-cesarean patients.
Seeing that practice become more targeted showed me that improvement is not only possible, but beneficial for both patients and providers. It meant better care, more thoughtful use of resources, and less unnecessary exposure to antibiotics. What stood out most was that change did not come from one person or one profession alone. It came from teams. Scrub nurses became more confident in speaking up about missing counts. Central Sterile Supply Department staff paid closer attention to sterilization indicators. Surgeons, anesthetists, nurses, and support teams began to see patient safety as a shared responsibility. The results could be seen in better compliance with safer practices and lower infection rates. But beyond the numbers, the impact was human: fewer complications, less suffering, and greater confidence that surgery could be made safer for patients and families.
My experience in Rwanda showed me that safer surgery is possible, even in resource-limited settings, when health workers are supported with practical tools, training, and the space to improve. It also showed me that antibiotic stewardship is not a separate conversation from patient safety. It is part of the same commitment to doing no harm. As we mark World Health Day, I hope we continue to recognize that stronger health systems are built not only through major investments and national policies, but also through attention to the details that protect patients every day. Safe surgery is one of those details. And from where I have stood, on the frontline of care, it can make all the difference.

About Roda
Roda Uwayesu is a theatre nurse and public health professional with 16 years of experience in surgical care. She currently serves as Lifebox’s Program Coordinator in Rwanda and is pursuing a Master of Public Health.