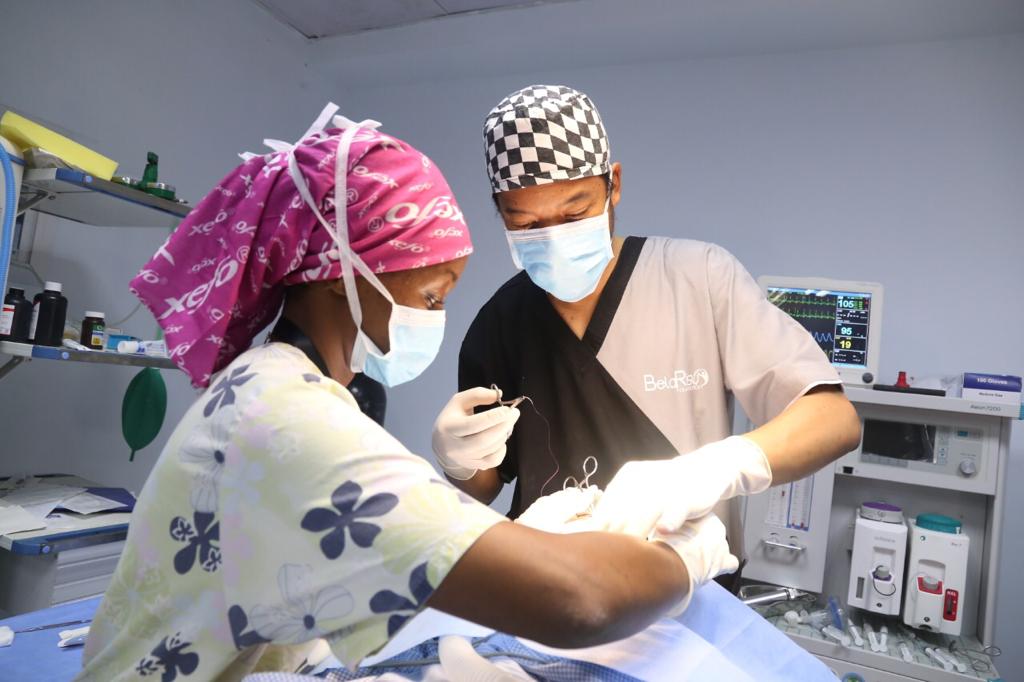
In the operating room where I work, there is an overlap between the roles of the surgeon, the anesthesiologist, and the nurses, with each team member being a leader in their own right. In my experience, the lack of training in teamwork and communication has led to risk of conflict, poor situational awareness, and respect, all of which can culminate in low-quality care that’s not centered to the patient’s needs at all. Assumptions are made, requests are ignored, and authority shunned – which can sometimes result in an unsafe environment for patient care.
It is no small issue when these problems appear in the operating room. I have seen the worst; maybe someone didn’t check the monitors because of an argument between a nurse and a surgeon. In such a situation, we can lose a patient with the flick of a hand. Or perhaps something is forgotten, like the surgical count, included in the course content for the Team CLEFT training manuals. I’ve seen cases when people were carrying out the surgical counts with no teamwork, no concentration, and nobody hearing anything. This can have dire consequences if, say, a throat pack is left inside a patient, and then once they’re awake they are deprived of oxygen, causing a threat to life. For these reasons, among others, it is beyond critical to have good teamwork in the operating room.
Before I came across Team CLEFT, I had never seen any sort of meeting or training addressing these key issues of teamwork and communication. When I met Team CLEFT through the Smile Train-Lifebox Safe Surgery and Anesthesia Initiative, and learned about how they are able to train healthcare professionals in quality, modern cleft care using structured training materials, I knew right away that I wanted to get involved.
The Team CLEFT training consists of different teaching methods, including simulation, videos, and live demonstrations.
The training impacts students in many positive ways. Most of them are aware of what is required of them, but they don’t necessarily know how to approach different challenges, such as conflict resolution. For example, through training with Team CLEFT, they learned how to approach a senior consultant for support in a conflict scenario. There are also some more practical benefits; students highlighted a better understanding of implementing important aspects such as surgery checklists, signing in and out of the theater, and how to use equipment such as the pulse oximeter. As a result of our training, they went out of their way to assure us that they would implement these improvements in their own institutions.
One of the most interesting things I observed when delivering the pilot training in Nairobi, Kenya was seeing the development of students from not knowing how to implement a skill to, following our demonstrations, being able to confidently complete a skill trial. When everyone knows their own role and the roles of their colleagues, it prevents assumptions being made that could cost lives. It also means that problems requiring attention or change can be identified much earlier, again increasing the quality of care.