
“The Challenges We Face Are Enormous”
An interview with Dr. Suleiman on the enormous challenges in Liberia in providing safe surgery and anesthesia.
 “Liberia is a country that faces enormous challenges in the provision of safe surgery and anesthesia for its five million people. There is not a single anesthesiologist in the country, although three are training in Nigeria. The anesthesia needs in the country are met by 80 nurse anesthesia providers. These providers are too few, often having to work across different facilities to meet the anesthesia needs, which means our workforce is exhausted. And while they do their best to care for our surgical patients, there is a big difference between a nurse anesthesia provider and an anesthesiologist in terms of training, understandably the knowledge base differs in terms of the response to problems.
“Liberia is a country that faces enormous challenges in the provision of safe surgery and anesthesia for its five million people. There is not a single anesthesiologist in the country, although three are training in Nigeria. The anesthesia needs in the country are met by 80 nurse anesthesia providers. These providers are too few, often having to work across different facilities to meet the anesthesia needs, which means our workforce is exhausted. And while they do their best to care for our surgical patients, there is a big difference between a nurse anesthesia provider and an anesthesiologist in terms of training, understandably the knowledge base differs in terms of the response to problems.
Our premier hospital is the John F. Kennedy Medical Center. It’s our biggest hospital and a teaching institution. It has eight operating rooms but of these, only one is active for general anesthesia. This has to be shared for any procedure that requires general anesthesia, whether it is general surgery, neurosurgery, orthopedics, plastics.
Another challenge we face is the lack of Intensive Care Units (ICUs). There is not a single ICU in Liberia, although one has been built but it has yet to be commissioned. With no ICU, most of the patients go back to the ward, and for those that need a high level of care we keep them in the recovery room for a longer duration. As an anesthesia provider it means we have no safety net if something goes wrong with the patient.
These are just some of the enormous challenges that we are facing here in Liberia. But we have to start somewhere to make a change and drive improvements.
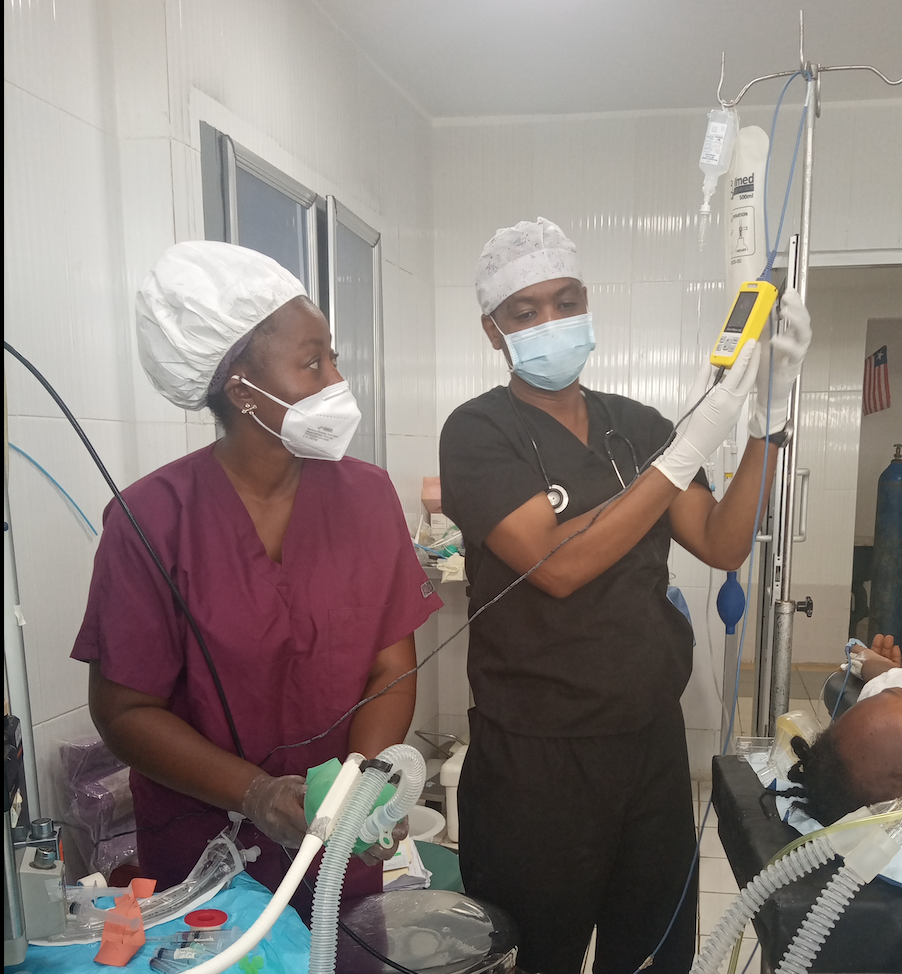
Surgery is not all about having a surgeon and a scalpel. We have to change this mindset. The surgeon and the scalpel are just one aspect. Safety is everything, and safety is the number one priority in anesthesia. The most important aspect of my work is showing how fundamental safety is in anesthesia.
The focus of medicine used to be around the doctor. The doctor decides what to do and when to do it, but the mantra has changed. Now the practice is patient-centered. Everything comes down to “does it benefit the patient?” What it means is that I have to be safe all the time.
My passion about patient safety started in 2014 when I was writing my dissertation during my residency training and I did some research on the WHO Surgical Safety Checklist. I realized that in Africa, we have not yet prioritized surgical teamwork and communication. Surgical teamwork and communication are the gaps that we need to fill in order to make surgery safe, especially in anesthesia. There is a very thin line between being a safe anesthesia provider and an unsafe one. One little mistake and your patient is gone. I always tell my trainees, never be in a rush to anesthetize a patient.
It is impossible to provide a safe surgery without a pulse oximeter. It is the basic minimum monitoring requirement for safe anesthetic and surgical practice. If you’re not using a pulse oximeter, you might be able to detect a problem, but by the time you recognize the problem, it may be too late for any intervention to save the patient’s life. There is no way that you can have a safe surgery without a pulse oximeter, it’s as simple as that.
The pulse oximetry gap in Liberia is wide, both in terms of availability and technical know-how. I am working with Lifebox to bridge that gap. We started our work at five hospitals with pulse oximetry workshops, giving the scientific background knowledge on how an oximeter works, how to troubleshoot some of the problems, and how best to interpret the results. By understanding how an oximeter works, providers understand why they need to use a pulse oximeter all the time.
Some of the centers in Liberia do not even have a nurse anesthesia provider to monitor the patient during surgery. The doctor gives the anesthesia then goes back to scrub, and also operates. This is not safe. We advise these centers that even if the person isn’t formally trained, they should have someone who is dedicated to anesthesia monitoring. The training that we are doing with Lifebox will help these types of providers enormously.
During one of the workshops, there was a discussion and some of the participants felt that the old style of just counting the pulse manually was a better approach to patient monitoring during surgery. I explained that the pulse oximeter allows you to detect the problem very early, and that early detection is the key. If the saturation starts to fall, you know that there is a problem. That is the best time to solve it. Not when the heart rate is low. Intervention may be late by that point. The participants were really excited by this and felt more empowered.
There’s a lot of work to be done in order to meet the pulse oximetry gap in Liberia, but I want to thank Lifebox for starting this work. Without Lifebox, most of these hospitals would not have pulse oximeters at all. And this is just the beginning. I am very excited for the future work ahead.”
Find out more about Lifebox’s work to support surgical systems in Liberia here.


