
Oximetry, Oxygen and COVID-19 in Lesotho: an interview with Dr. Eric McCollum
Pediatric pulmonologist, Dr. Eric D. McCollum discusses oximetry, oxygen and Lesotho's COVID-19 response with Lifebox.
Dr. Eric D. McCollum is a pediatric pulmonologist at Johns Hopkins School of Medicine based in Lesotho. Dr. McCollum has partnered with Lifebox on a range of patient safety projects since 2011, including improving care for pediatric pneumonia through pulse oximetry and developing an innovative pulse oximeter probe for children under the age of five. Most recently, Dr. McCollum has partnered with Lifebox to develop tools and guidance on the use of pulse oximeters in COVID-19 care and to distribute 50 pulse oximeters in Lesotho as part of Lifebox’s COVID-19 response, supported by ELMA Philanthropies and UBS Optimus Foundation.
Lifebox talked with Dr. McCollum on pediatric pneumonia, oximetry and COVID-19 response in Lesotho.
“Pulse oximeters, if deployed effectively at all levels of the health system, can be an objective tool to identify higher risk or more severely ill people with COVID-19. In a country like Lesotho that lacks intensive care resources, early identification is paramount for people to have the best possible outcomes.” Dr. Eric. McCollum, Pediatric Pulmonologist at Johns Hopkins School of Medicine.
Please introduce yourself and your work in pediatric pneumonia. 
My name is Dr. Eric D. McCollum and I am a pediatric pulmonologist at Johns Hopkins School of Medicine. I’m the founding director of a program at Johns Hopkins called the Global Program in Respiratory Sciences and I’ve been based in the small sub-Saharan African country of Lesotho for the past four years. I’ve collaborated with Lifebox since 2011 when we worked together on a project in Malawi using Lifebox pulse oximeters for the care of children with pneumonia. Since then I’ve collaborated with Lifebox on several projects, including developing an innovative pulse oximeter probe.
I lived in Malawi for five years after completing my pediatric residency training and worked as a pediatrician at the government referral hospital in the capital city Lilongwe. I became increasingly interested in pediatric respiratory disease in low-income and middle-income countries, an interest that developed largely from my daily struggles caring for the overwhelming numbers of children with severe respiratory illnesses in the hospital. I came to learn that child pneumonia was – and continues to be – a major public health problem that is under-appreciated. It is the leading cause of infectious death among children below five years of age globally, and the vast majority of these deaths occur in low-income and middle-income countries. In an effort to improve outcomes of children with pneumonia and other respiratory illnesses, I wanted to better understand the implications of pulse oximeters and hypoxemia along with potential therapies like oxygen and non-invasive ventilation. I returned to the US and completed additional training in pediatric pulmonology and have continued to live and work in resource-constrained settings thereafter. I have subsequently lived in Bangladesh, Lesotho, and, currently, South Africa. My work has evolved over the years to be a mix of clinical care, clinical research, and education and training, all focused on the respiratory health of children in low-income and middle-income countries.
How has COVID-19 affected this work? We hear about the ‘double burden’ of pneumonia and COVID-19 – could you explain this for us?
COVID-19 has turned everything sideways in all respects. The indirect effects of the COVID-19 mitigation measures (i.e., lock-downs, school closures, mask wearing, hand hygiene, etc.) have quite dramatically reduced the burden of respiratory illnesses, including pneumonia, among children. This is a relief. Fortunately, COVID-19 doesn’t seem to directly impact children as much as adults, and this is really a blessing. That said, there are real concerns that given the economic impact that COVID-19 is having, that we may observe a lagging increase in malnutrition, coupled with reduced vaccinations, and this may cause a substantial increase in child pneumonia later in the pandemic as countries open up and schools re-open. We’ll have to monitor this closely.
As the only pulmonologist in the entire country of Lesotho, I’ve had to do my part and assist the government in their COVID-19 response. I have needed to switch my focus from children to adults for the pandemic. As we began assisting in the pandemic response it was not surprising to find that the health system lacked adequate oxygen treatment as well as pulse oximeters to detect hypoxemia (low blood oxygen) for adults also. This has been a chronic problem in the child pneumonia space. Although we’ve worked hard through donors to try and address these systemic issues, the double burden is that COVID-19 is placing extreme, added pressures on oxygen needs in health systems like Lesotho that have to date not prioritized their oxygen systems. So, if we do see a return of pediatric respiratory illnesses like pneumonia we can expect further strains on the systems needed to detect and treat children with pneumonia and adults with COVID-19. Hopefully this will not happen.
What are the wider ramifications of the COVID-19 pandemic?
 The COVID-19 pandemic is impacting all aspects of our lives as everyone sees on a daily basis, from the economic impact to the health effects – it’s everywhere. The positives in Lesotho is that this pandemic has perhaps for the first time shown a light on the need for a functional oxygen system. The focus to date over the past 15 or more years has been on HIV and more recently TB. This focus has not addressed more basic aspects of the health system like oxygen. So there has been an influx of resources over the past six months to quite rapidly address the lack of oxygen in Lesotho and we’ve worked hard with our partners, donors, and the Ministry of Health to get these resources out across the national health system so that people sick with COVID can access oxygen if they need it.
The COVID-19 pandemic is impacting all aspects of our lives as everyone sees on a daily basis, from the economic impact to the health effects – it’s everywhere. The positives in Lesotho is that this pandemic has perhaps for the first time shown a light on the need for a functional oxygen system. The focus to date over the past 15 or more years has been on HIV and more recently TB. This focus has not addressed more basic aspects of the health system like oxygen. So there has been an influx of resources over the past six months to quite rapidly address the lack of oxygen in Lesotho and we’ve worked hard with our partners, donors, and the Ministry of Health to get these resources out across the national health system so that people sick with COVID can access oxygen if they need it.
Could you talk to us on the work you are doing in responding to COVID-19?
As I mentioned, prior to COVID there had been very little emphasis placed on having robust oxygen systems across the hospital system here in Lesotho. So this has been our focus. I’ve worked with Jhpiego, a public health affiliate of Johns Hopkins, here in Lesotho through support by USAID to assist the government of Lesotho in their COVID-19 response.
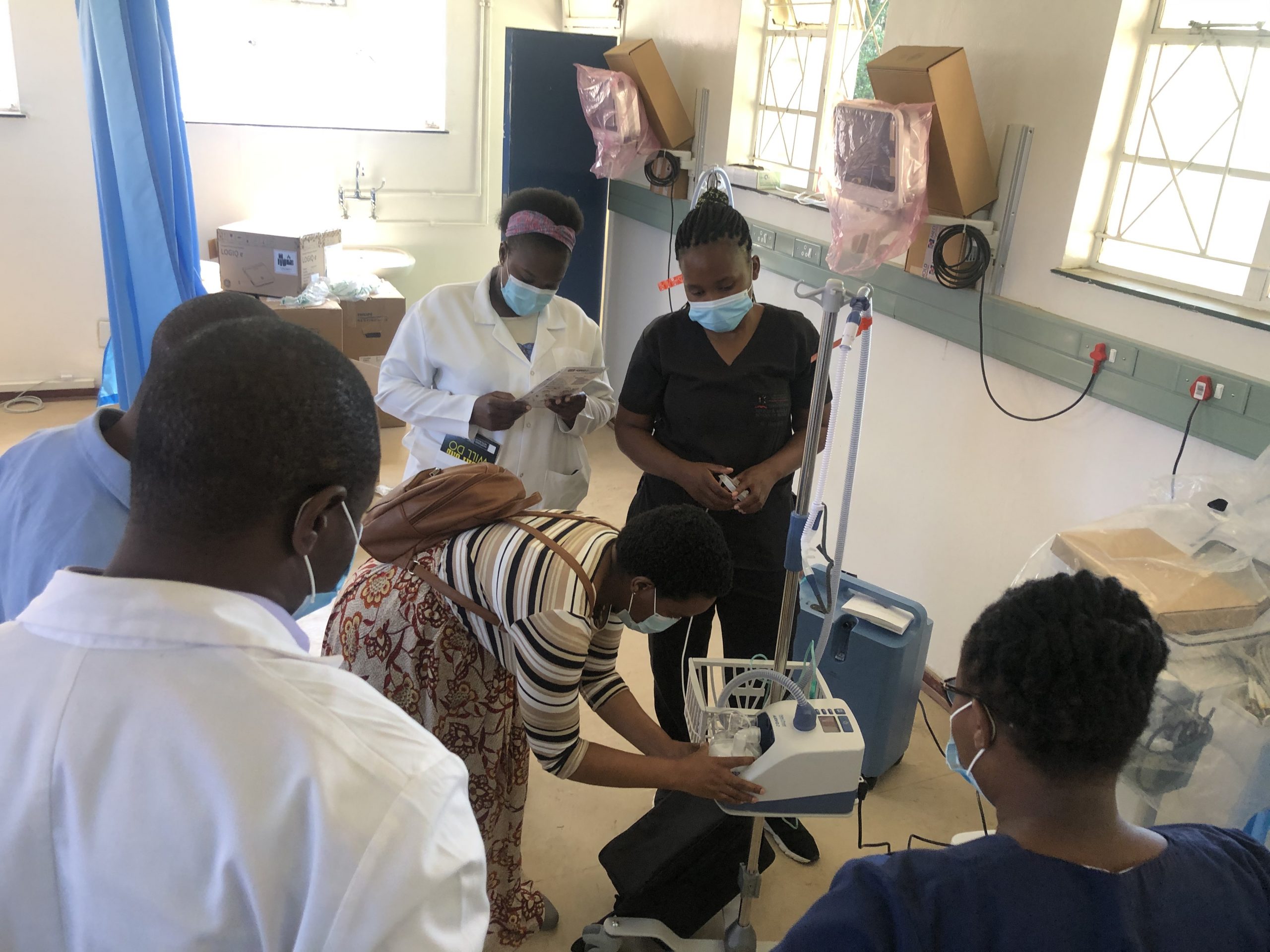
We’ve worked to set up two COVID-19 treatment centers as well as distribute and train healthcare providers on using pulse oximeters, oxygen concentrators and cylinders, and heated high flow care units. We’ve trained over 2,000 healthcare providers on the country’s COVID-19 case management guidelines and more than 125 providers at the treatment centers and other hospitals on advanced respiratory care.
During the first wave of the pandemic, which went through August 2020, we provided in person case management support at the treatment centers to physicians and nurses caring for patients sick with COVID-19. Lifebox generously donated pulse oximeters to Lesotho and we distributed them to all hospitals and trained providers on using them. Given the vast majority of hospitalized COVID patients can improve with oxygen, we really wanted to focus our efforts on getting oxygen up and running and to be more sustainable. Then we can build more advanced care on a more solid platform. Although there was an early focus on mechanical ventilation, patients cannot be effectively mechanically ventilated without oxygen. So we needed to start there. Lesotho fortunately doesn’t suffer from widespread power outages and this means that oxygen concentrators are a good fit for their system.
“There’s a very real opportunity for Lesotho to build a functioning oxygen ecosystem with pulse oximeters and sustainable oxygen supply, and this would be a fantastic legacy of the pandemic.” Dr. Eric McCollum
 You have previously partnered with Lifebox on improving oximetry for use in pediatric patients. What is the role of oximetry in the COVID-19 pandemic – why is it proving to be such a valuable tool for healthcare providers working during this pandemic?
You have previously partnered with Lifebox on improving oximetry for use in pediatric patients. What is the role of oximetry in the COVID-19 pandemic – why is it proving to be such a valuable tool for healthcare providers working during this pandemic?
In my view pulse oximetry is one of the key centerpieces of the COVID response. Pulse oximeters serve to identify those people with more severe COVID disease, which is largely characterized by a low oxyhemoglobin saturation. Early and objective identification of these cases can help healthcare providers guide people down the best care pathway for them so that they can not only access oxygen but also receive hospital level care when needed. Without pulse oximeters these decisions are made more subjectively, less effectively, and typically later in the disease course when disease severity may be more obvious but patients may be less responsive to available treatment. So pulse oximeters, if deployed effectively at all levels of the health system, can be an objective tool to identify higher risk or more severely ill people with COVID-19. In a country like Lesotho that lacks intensive care resources, early identification is paramount for people to have the best possible outcomes.
With the world still very much in the grips of the pandemic, what is giving you the most hope when you look at how we are responding to the pandemic?
Vaccines. My hope is wrapped up in the gift science has given the world – highly efficacious vaccines. The production and distribution of vaccines will be extremely challenging but can be achieved if we put our minds to it. My other hope is that pulse oximeters and oxygen resources are finally getting the attention that they deserve and have a lasting legacy in countries like Lesotho that previously lacked these precious tools and therapies.

