Front Page Togo
From the instant of publication in 2005, ‘Deaths Associated with Anaesthesia in Togo, West Africa’ was famous.
We knew that anaesthesia in a low-resource setting could be dangerous – that without the equipment, support and training safety hallmarks of higher-resource colleagues, patients were at increased risk.
But Fatou Ouro-Bang’na and colleagues gave us a number, showing that the risk of anaesthesia mortality could be as high as 1:133.
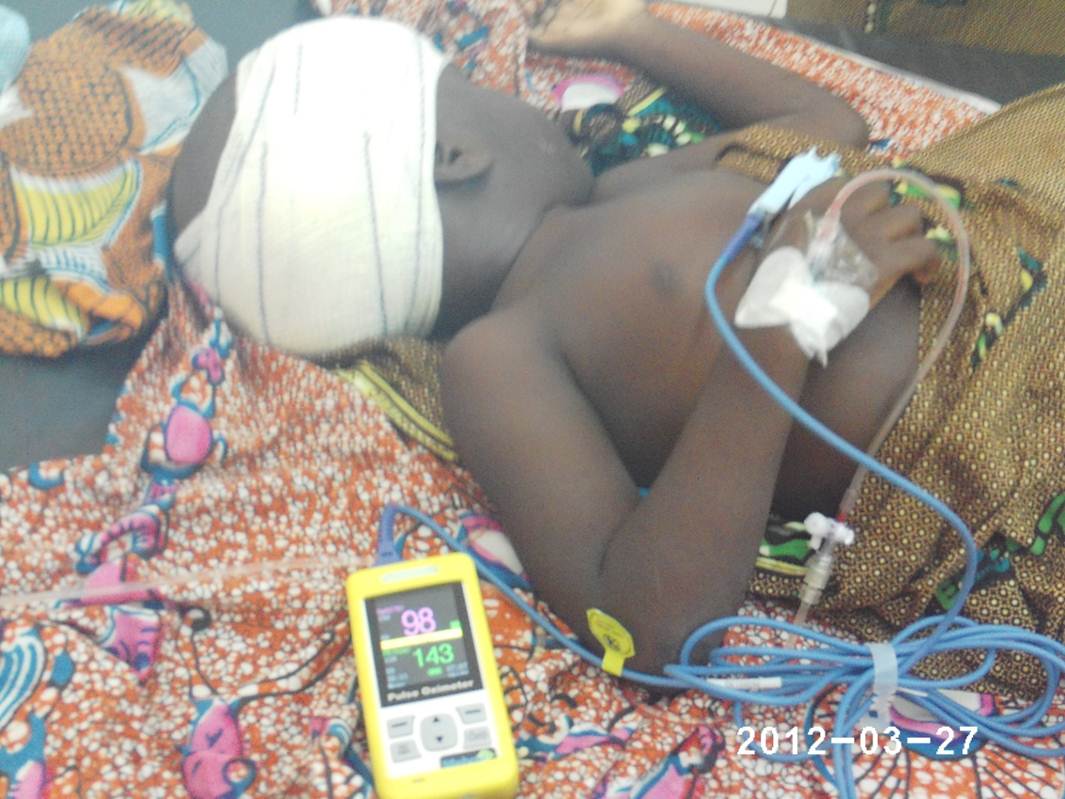
15 out of 26 hospitals did not have a single pulse oximeter.
“In Sub-Saharan Africa particularly, there are not many studies,” the anaesthetist explained in the BMJ. “This means that sometimes people don’t know what exactly is happening in their own countries. People asked me, why are you publishing this? Are you sure that it is true? I chose to make it known, not just to anaesthesia providers in Togo, but around the world.
And once we have the numbers we can be better at addressing the problem.”
It’s been cited more than a hundred times since.
In the last few years, we’ve been proud to work with Fataou and Togolese colleagues to push back against these numbers, provide pulse oximeters and training to hospitals across the country – and this month they’re back in the academic spotlight.
“Incidence of hypoxia and related events detected by pulse oximeters provided by the Lifebox Foundation in the maternity unit at Sylvanus Olympio University Teaching Hospital, Togo” was published this month in the Journal of Anaesthesia.
An audit of 540 surgical procedures over 3 months, it gives snapshot of birth, life and risk in a Togolese maternity unit, and reviews the impact of improved oxygen monitoring.
It’s not a perfect picture – with more than 70% of patients emergencies, and resources still strained, anaesthesia mortality and cardiac arrest still play a devastating part.
 But we can see that there’s positive change.
But we can see that there’s positive change.
“Lifebox pulse oximeter enables detection of hypoxia in patients undergoing surgery.” With monitoring, there’s a chance for anaesthesia providers to react, to take resuscitative action. To turn those numbers around.
This is hugely exciting, and we hope that a paper showing positive improvement gets as much attention as one that shows a realistic but negative truth.
Anaesthesia mortality in higher-resource settings is roughly 1:200,000. The global gap in lives safe and lives lost is appalling, and there’s a lot of work to do.
But Hamza Sama, Fataou and all the anaesthesia providers who have their hearts in the operating room – and their eyes and ears on a pulse oximeter – are devoted to their countries, their colleagues, their hospitals, their patients. They’re going to go the distance.
And we should follow their lead – they’re the ones who were brave enough to show us how far we have to go in the first place.