The Long and Winding Road (to surgical safety)
If you can’t get to hospital, you can’t get an emergency caesarian section, or life-saving surgery after a road traffic accident. If supplies or engineers can’t reach the hospital, drugs will run out and equipment will break. Healthcare providers are forced to make terrible choices between treatment and unsafe care:
“I am a junior anesthesiology professional who works in a district hospital,” Abayehu Haile wrote to us recently. “It is found 455km away from the capital city of Ethiopia. Even though it is a district hospital, it serves more than 500,000 people living in four surrounding districts.
“In this hospital there are so many challenges to work because of resource limitation. Pulse oximetry is the heartbeat for my work. But the only oximeter we had was always on and off in its function. It was really hard to work with this monitoring and to have safe surgery, but I had no choice – as an anesthetist I am striving to save life as much as I can.
“It was not easy to say ”this monitoring needs maintenance” and stop work. Most of our patients can’t go to Jimma University Hospital, which is found 75km from this town. They don’t have enough money to pay for further transport and their only choice when we said no was to go back to their home with pain. So as a professional it was difficult to cancel cases because of monitoring and am sure you can understand how many challenges were there.”
The logistics of arranging and arriving at a training workshop are significant – but get it right, and the impact will be felt for miles around.
So we were thrilled to hear that Operation Smile, an international charity that provides free cleft palate surgery in low-resource settings, was planning an education workshop in the southwest city of Jimma in March of this year. Action stations…
We worked closely with the Ethiopian Association of Anaesthesiologists (ESA) to make sure that anaesthesia providers from all around Jimma were able to attend the workshop; we got generous permission from the Ethiopian Ministry of Health to import oximeters without customs charge; we strategized with Operation Smile to find space for the Lifebox training workshop in their packed schedule, and in early February we shipped 31 oximeters to their office in Addis Ababa. The Operation Smile team whisked them out of the airport and southwest to Jimma, 300 km away, and…smile!
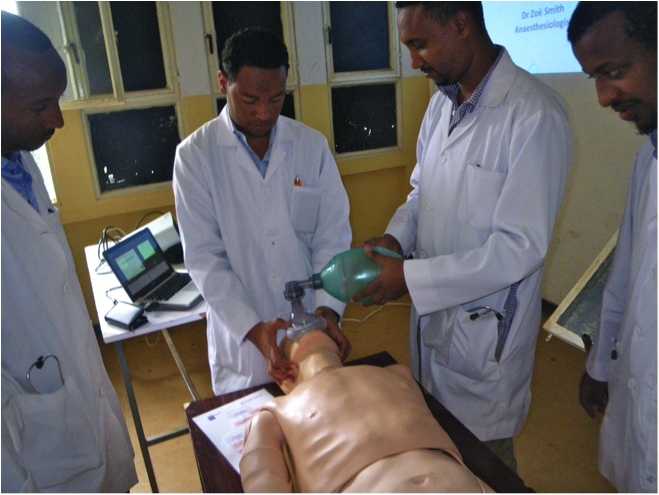
Pulse oximeter recipients at the Lifebox training course run by Operation Smile in Jimma, March 2012
More important than the pictures, of course, is what happens once the cameras are off.
The rare opportunity for anaesthesia providers to meet gave them an opportunity to swap stories with the only other people who really understand the day-to-day realities of their work. “When we shared ideas, I observed that every professional was facing challenges,” said Abayehu.
Meanwhile, the training and equipment make an immediate difference: attendees returned home with the monitoring they needed for their surgical patients, and a better understanding of how systems like the World Health Organization’s Surgical Safety Checklist can make a life-saving difference to their patients and practice.
But the path to surgical safety can be longer and lumpier than the road to Jimma. We’re not done teaching and learning from our colleagues. Dr Zoe Smith, a British doctor, recently arrived at the University Hospital, where she’ll be working as an Operation Smile visiting lecturer for the next few months. She’s following up on the Lifebox pulse oximeters and helping to implement the WHO Surgical Safety Checklist, and we can’t wait to tell you how well it’s going so far – but you’ll have to wait till next time.
She’s already put up some road signs.