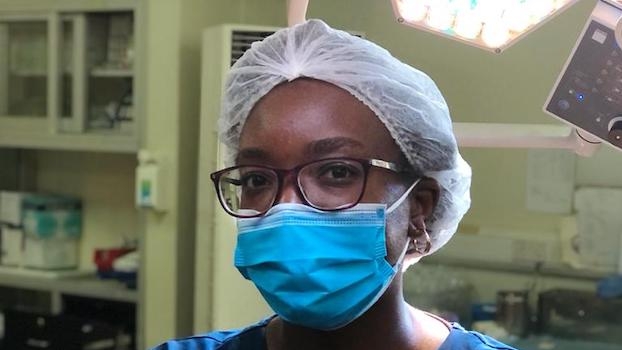
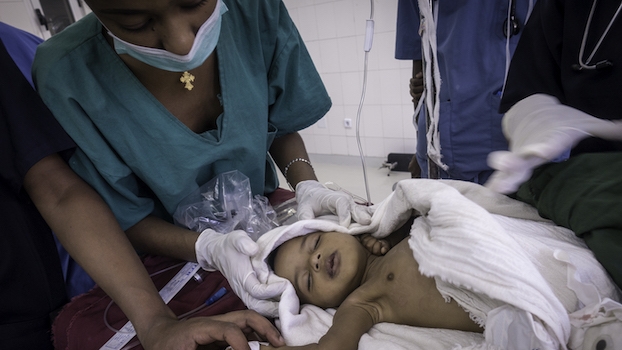
Clean Cut (adaptive, multimodal surgical infection prevention program) for low-resource settings: a prospective quality improvement study
This study showed that Lifebox's Clean Cut program improved infection prevention standards to reduce SSI without infrastructure expenses or resource investments.