Tanzania, safe surgery with safe anaesthesia
Lifebox has a long history of working with colleagues across Tanzania: from supporting anaesthesia providers with essential equipment to collaborating with international and local partners such as the Society of Anaesthesiologists of Tanzania (SATA) in delivering training workshops.
So we are delighted to share the interview below with German doctor, Daniela Kietzmann who works as a visiting anaesthesiologist in South East of Tanzania. Splitting her time between the two regions of Mtwara and Lindi that lie close to the Mozambique border, the facilities that she supports are more than 500km from any other hospitals where patients could be referred to. Here she tells us of her commitment to “safe surgery with safe anaesthesia for everybody” and the difference Lifebox is making on the ground.
What changes have you seen in surgery and anaesthesia since you’ve been working in Tanzania?
I went to Tanzania for the first time in January 2009 and stayed one year. Since then I have returned each year for eight to twelve weeks. I was the first anaesthesiologist to visit the hospitals of St Walburg’s District Hospital in Nyangao, Lindi and St Benedict’s Referral Hospital in Ndanda, Mtwara that were founded by Missionary Benedictines from Bavaria, Germany, more than 80 years ago.
Most of the surgeons are assistant medical officers and have not completed a formal specialist training. In spite of this, they have learned to perform different and increasingly difficult operations. In Nyangao, a Tanzanian Benedictine nun was sent to Mwanza for three-years specialist training as a surgeon. Many patients are referred from surrounding small hospitals late, often too late. We experienced several tragic deaths of young patients who could have been saved if they had reached Nyangao Hospital earlier.
Yet in spite of the limitations many patients’ lives are saved thanks to careful monitoring and observation of the patients. I will never forget our very first patient for the new ICU in Nyangao in October 2011, five- weeks-old Yasiri who came with obstructed inguinal hernia. Our surgeon Dr. Jankiewicz had to perform an extended operation with resection of gangrenous intestine and then reoperation two days later. Yasiri survived even that operation and anaesthesia. After three days the little boy had lost 20 % of his body weight, but then he was able to start breast feeding and recovered without complication. Of course, that case was extremely motivating for our nurses. They knew very well that such patients had not survived in former times.
Nurse Scholastica with the new Lifebox pulse oximeter at St Walburg’s
What challenges do the two hospitals you work in face?
There are so many electrical power cuts and voltage fluctuations that much equipment is not long-lasting. At St. Walburg’s Hosptial all the pulse oximeters except the Lifebox pulse oximeter stopped working one by one. No spare parts were available. There’s also sometimes no running water, lack of oxygen, lack of vital drugs, lack of laryngoscope, tubes, laryngeal masks, pulse oximeter, automatic BP monitor, ECG monitor.
The lack of professional training for many members of staff is a challenge – one person giving anaesthesia alone without having had formal training for anaesthesia.
Anaesthesia is provided by nurses, and often these nurses are just trained on the job. Anaesthesia diplomas like the one at Kilimanjaro Christian Medical (KCMC) make a great difference since the alternative is to give anaesthesia without any previous formal training. The quality of the training KCMC is excellent. It is amazing how much the nurses learn during one single year at a teaching hospital.
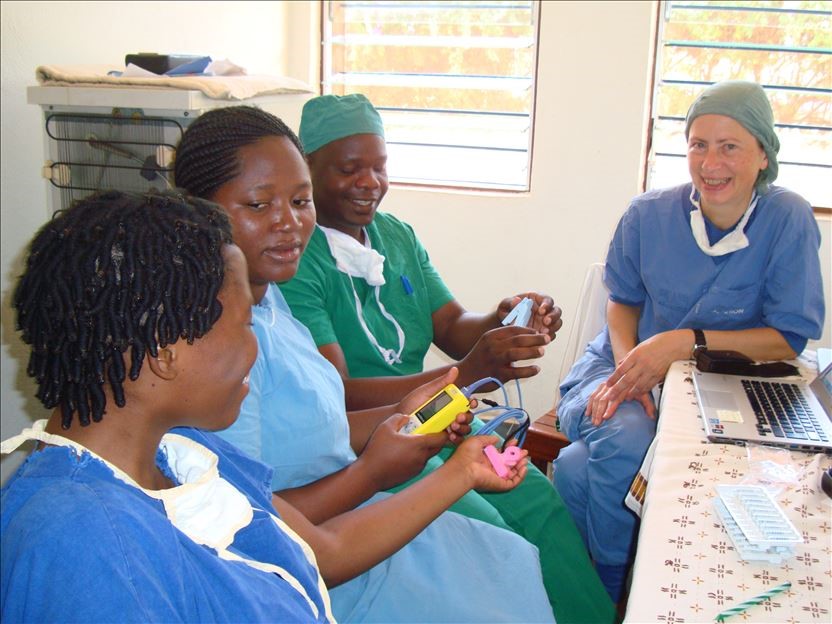 Dr Kietzmann training three anesthesia providers trained-on-the-job – Samson, Sylvia, and Agnes – with the new Lifebox pulse oximeter at Ndanda Hospital.
Dr Kietzmann training three anesthesia providers trained-on-the-job – Samson, Sylvia, and Agnes – with the new Lifebox pulse oximeter at Ndanda Hospital.
What difference does Lifebox training make?
At St Walburg’s the doctors organised a Lifebox workshop, announced at all wards and departments and even in several small surrounding hospitals. There were 90 participants so we had to carry out two sessions. Each group consisted of nurse attendants, ward attendants, enrolled and registered nurses, anaesthesia and ICU nurses, clinical officers, assistant medical officers, medical officers and even doctors in charge and all surgeons participated.
When anaesthesia providers really understand the meaning and importance of oxygen delivery, blood pressure, pulse, breathing, oxygen saturation and how to keep them within margins, and how to recognise and to intervene in a critical situation, this makes a very great difference for the whole work that they are providing. Lifebox training is effective and I am convinced that proper Lifebox training can save many lives. I realised that I should repeat a workshop every year, even at Ndanda Hospital too.
 Dr Makota, gynaecologist AMO from Nyangao instructing nurses
Dr Makota, gynaecologist AMO from Nyangao instructing nurses
What do you find rewarding about going back to work in Tanzania each time?
It is simply my vocation to work as an anaesthesiologist where I can and where I am needed most urgently. I was and am the only anaesthesiologist regularly visiting and working in South East Tanzania as far as I know. I love the people, I have good relations to the Tanzanian anaesthesia nurses at the hospitals I am visiting each year and they ask me to return each year and we have a lot of fun with one another. I hope for access to affordable, basic, safe surgery with safe anaesthesia for everybody.


