“That’s why I’m always advocating for teamwork”
Discussing patient safety in Ethiopia and improving surgical teamwork with Lifebox Global Clinical Director Dr. Negussie and Global CEO Kris Torgeson
Kris Torgeson: I’m so pleased to be here today with my wonderful colleague, mentor and friend, Dr. Tihitena Negussie who is an amazing pediatric surgeon working in Ethiopia. She has joined Lifebox as our Global Clinical Director and we’re absolutely thrilled to have her.
Dr. Tihitena Negussie: I’m Tihitena Negussie. I am a pediatric surgeon and have also been a general surgeon. I was working in Black Lion Hospital. I’ve been in Black Lion for almost more than 20 years since I started my medical education and as a staff working there, I have spent more than 14 years there. I have a lot of experience working there, whether they are positive and negative, they changed my life. They showed me how to handle things and also it helped me how to live with friends and colleagues.
Kris Torgeson: I wanted to ask you as I always have to ask anyone who’s gone into the medical field that what first inspired you to study medicine. Was there a certain moment where you just knew that you had to become a doctor? And then how did you get into surgery?
Dr. Tihitena Negussie: Once I joined Addis Ababa University, it was the first year that we chose which field we are going to pursue for the future. I decided to join medicine because during the introduction, colleagues coming from these different universities and telling that the different things that we can achieve by joining medicine, engineering, pharmacy. So as a person coming from the medical school has got some kind of convincing talk, so I just decided that I think I better choose medicine and I communicated with my families whether I chose the right thing or not and they say, they are always 100% with me, so I joined medicine. And during my stay, I had the best time and I saw how we can change people’s lives with simple intervention, how we can help the needy people. So that’s why I said medicine is the right choice for me and I will be there for people who needs me so I was happy joining that. And then during my stay in medical school, all departments are good, but, you know, surgery. One thing I was saying I am going to suture any wound that my father is going to have and the other thing is the art, the teaching environment, the different kind of interesting cases that the surgeons are doing, and the surgical field totally changed my mind that I’m not going to do any specialty except surgery. That’s why I pursued the general surgery. And the most important thing, why I chose pediatric surgery? I know I didn’t decide which subspecialty I would pursue while I joined surgery, but once I joined surgery, the fact that the kids are there to get the service and the pains that they are passing through, even including the family’s pain, and once you give them the service, their innocent face getting like excited and them being happy makes you like that so I can change their happiness with like a minimum service I can give them. And I can save their life for the future by just doing the best practice that is expected of me. And also the shortage of the professionals in that field and the burden they are going to have, if I’m there, I’ll be there for sharing their burden and changing the environment that we are working in. So that’s why I started medicine and ended up being a pediatric surgeon.
Kris Toregson: How did you first get into the issue around patient safety? It’s something that is obviously the core of Lifebox’s work as we’re born out of the patient safety movement at World Health Organization and I know your dedication to it. I wondered if there’s any moment where you really recognize that more needed to be done in Ethiopia and elsewhere around patient safety.
Dr. Tihitena Negussie: The first frustration that I faced was when I was a resident, as being a country– living in low and middle income countries, there is infrastructure shortage, there is equipment shortage, it was obvious. But in addition to that, the attitude towards not being able to solve a problem because there is no equipment, there is no infrastructure grows bigger and bigger and the fact that human resource impact over changes in the environment is not seen in the operation theater I was practicing.
So there were times we lost patients intraoperatively because the patient was not properly monitored because we didn’t access pre-operative checklist or sign in with the WHO Checklist or just simple checklist, and the machine was not working intraoperatively and the patient got arrested and died. That was– you know, losing a patient on table is a nightmare for a surgeon. So it will traumatize you and sometimes you will be away from the OR for days, months, you might not get back to the OR because on-table death is frustrating.
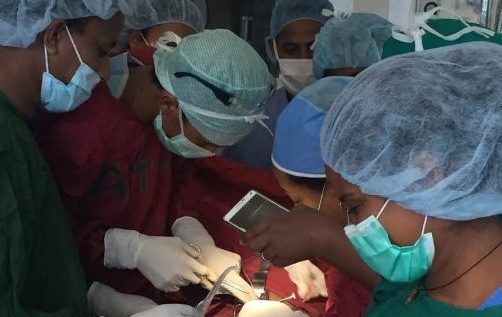
And sometimes because of this equipment shortage like light outage. I had a patient who bled intraoperatively. While we were doing the surgery, in the middle of the surgery, the light was off. So the electricity went out. It went out, there was no backup generator, and we were cutting a vessel. Just when we cut the vessel, that light is off and we couldn’t access the vessel easily and the patient was bleeding. We tried to pack. Fortunately, the colleagues who were just watching the surgery was using their mobile battery to help us out. So when I see those things, it is not the environment that I should work in for the rest of my life. And I said I should be part of the person who is going to change this kind of environment. And those are the moments that made me think patient safety is an issue. And when this kind of things come to pediatric surgery, specifically when it comes to the pediatric operation, it is so much traumatizing because knowing that it is a preventable issue, knowing that 50% of the complications can be easily prevented by just following the standards, and causing this kind of complication to the baby will make the baby’s or the patient’s life miserable and it will give the family, the country, to break their hope for the future. So it shouldn’t be a traumatic site for the patients coming and getting the service. There should be an environment where they can get the service as much as they deserve it, as much as they need. So that’s why I say, no, we have to play a role and we have to be there for changing these kind of environment and then we have to talk about patient safety as much as possible with the capacity that we have got.
Kris Torgeson: If you talk about what areas need to be addressed to improve patient safety along the lines of what you have just described. So you’ve said it’s not necessarily the equipment, it’s not necessarily having more staff, it’s not necessarily having, you know, mentors there, etc., but it’s really things that you can do. What are some of the key elements that you think need to be addressed and that you’ve been working to address in patient safety?
Dr. Tihitena Negussie: In all things, if you are working with a good team, a great team, you will end up identifying this problem and you will propose the easiest solutions that should be implemented. So when I was OR Director in Black Lion, the most difficult thing for me to manage was managing conflicts between colleagues. As you know, as a human being, we are good at complaining. We are good at fighting. But we don’t want to take the initiative to solve those kind of fighting or those kind of conflicts. So, I was just sitting in my office one day and think to myself that so if I can approach these groups, even like I can approach my colleagues working in the OR, then how can they be part of the solution than just expecting somebody else to make them a solution?
So the most important thing that crossed my mind is working as a team and building up a good team works wonders in the OR. So by that the things that I can’t see will be seen by my colleague and the things that cannot be seen by my colleague can be seen by me. So one important factor in changing the safety of the environment is sitting together, thinking together and proposing solutions together. So working on teamwork. That’s why I’m always advocating for teamwork.
Kris Torgeson: How would you define the role of global surgery and the partnerships that are created? How do they help or what do they get right, what can be improved on how they work with someone like yourself who’s really dedicated to improving patient safety?
Dr. Tihitena Negussie: So by definition, when we say global surgery, it is just a rapidly developing multi-disciplinary field by aiming to achieve the best service which is safe and also accessible to all working in the whole world health system. So when we say that to make things globalized, you have to have a good connection with members working in different units of the same institution, colleagues working in different hospitals of the same country, and also colleagues working in different hospitals of the world. So this kind of relationship will help you to know the different attitudes, the different perspectives towards the surgical field that you have to work in. I got the chance of getting training in some parts of the world, both in low and middle income countries and to the high-income countries, and I saw different infrastructures, different systems, different kinds of human resource capacities, number wise and also knowledge wise. And having this link helped me to appreciate the difference we have got and the lessons we can take from these experiences and continuing my communication with these colleagues helped me to strategize what things should be taken to improve my hospital’s functionality. So I still keep on communicating with these staffs and I still communicate with them whenever I have difficulty, even in my surgical practices, and also not only the surgeons working there, I start communicating with the nurses working in the OR, even the anesthesiologists working in the different hospitals so that they can help me with the system they are using, and using it for my institution. So this kind of communication is an important factor for me to improve, but the fact that you didn’t go abroad and get the training doesn’t mean that you are not global. You can continue your communication with the colleagues working around you and you can share their experiences. So this is the most important thing we need to know about globalization because whenever we are talking about this kind of thing with your colleagues, some of them will complain that you got the chance of like seeing that kind of facilities, so I’m not the one who is going to work with you. So you have to convince them that the fact that I’m having this kind of experience will help us to improve and the fact that he is having that kind of experience will help me to improve my practicality. So you don’t have to always get involved with this kind of situations to change your environment.
Kris Torgeson: I wondered if you could talk a little bit about the importance of the World Health Organization Surgical Safety Checklist and why even when you hadn’t had formal training on it, you recognized that it could be a useful tool. Maybe just describe for people what it is and why as a surgeon, you saw it as a valuable tool. How can it help?
Dr. Tihitena Negussie: When using the details of the Checklist, it is a simple standard which you know, which you have learned while you were taking the training during surgery, during anesthesia or during nursing, but it’s just knowing and following that nothing is missed from that part will help you to decrease your avoidable or unnecessary complications you are going to face during surgeries.
As I told you earlier, there was one patient who we lost because we didn’t properly monitor the patient intraoperatively because we didn’t check that the monitoring was properly functional before we started the surgery. So this kind of things can be easily avoided if you use the Checklist properly. And it is just following the simple standard.
Kris Torgeson: If you consider the role of the surgeon in surgery as we always know is so core and if you watch medical TV shows, it’s always the surgeon who rules. But we know that it’s really about the team as you’ve said already. How important is it that you as a surgeon and leader of the team create an atmosphere where there is open communication, etc.?
Dr. Tihitena Negussie: For the first time where I was planning on pushing on the teamwork, it was somewhat difficult because most of our nurses are somehow shy and they’re not outspoken and most of the surgeons are over dominant, and even anesthesiologists are over dominant and they want to also be the leader, so the leadership is literally want to be owned by either the surgeon or the anesthesia team.
So when I started advocating about the team thing, the most important thing that I did is starting to ask the nurses to give their comments, I start asking the nurses what things they want to do and where to act, and I try to convince my colleagues that everybody has got a role and the responsibility depending on their field. If one of the team member is not there, the OR is not going to be safe.
So we are not going to function as far as we are not respecting each other and we are not using our colleagues’ capacity because our colleagues’ capacity and input will boost our functionality. And as the proverb says, “one hand can’t clap.” So as a surgeon, you are not going to do the surgery and as an anesthesiologist, you are not going to do the surgery. So you have to have a nurse, you have to have anesthesiologist, you have to have a surgeon, so all of us should be there to have a surgery and we have to have a backup of even the cleaners, the biomedicals, the OR technicians so nobody is a leader by himself and everybody is a leader for everything. So depending on the scenario, everybody should take the leadership role; depending on the activities, everybody should propose an idea or solution. So we don’t have to give ourselves more value and look down to our colleagues.
Kris Torgeson: Before we close, I wanted to hear a little bit about your role of Global Clinical Director for Lifebox and this has responsibilities not only in Ethiopia, but also in our other programs around the world I wanted to ask what attracted you to taking this challenge on and what do you hope to achieve during this year? And I hope we can have another conversation midway through and check in about it.
Dr. Tihitena Negussie: I am really happy that I joined Lifebox officially. I was there for almost more than three years, but I’m now officially hired, so I want to work hard with my full energy to achieve my objective sets while I’m joining Lifebox. So the most important thing is I want to change the culture and the system of OR environment in my country, especially for things like in the specific operation theater, not only to the surgical department, but all the staffs working in the OR; their system, their culture should be changed so that everybody will function together to come up with a better outcome to the operation theater and not only the infrastructure issue, but also the attitude of human resource can have a similar impact on improving or deteriorating the functionality of operation theater. So we have to work out what is expected of us, then we can convince that as a country, as an institution, to go to make an input on the infrastructure, but if we are not doing our part, we are not in a place to ask for more.
So we have to change ourselves, we have to work on more team spirit, we have to work more on solutions than complaints, then we have to bring up a change on the system of our operation theater. Once I’m good in achieving this, I want to expand it to the world, especially in those low and middle income countries should share our experience starting from the scratch and change their surgical world so that they will have the best practice in their sites or environments they are working at. And additionally, as a pediatric surgeon, I want my kids to have the best service they deserve to have because as being kids, you don’t deserve to pass through challenges. So having the disease is a challenge, it is a pain and having unnecessary suffering because of the environment that you are getting the service is not fair. So we have to offer them the best service they should get by simply changing the working environment, by simply changing the system of the operation theater in the surgical ward.
Kris Torgeson: There’s no better note to end it on than your dedication to ensuring that children like your own and others in Ethiopia and around the world can have the best care possible when they need it and without them having to even think about it or their parents to worry about it. So I am just so delighted to have spoken with you today as I always am, Dr. Tihitena, and I’ll really look forward to continuing the conversation and hoping that we can check in again at some point.
Dr. Tihitena Negussie: Thank for having me as part of you. Thank you so much.
Find out more about Lifebox’s work to improve the safety of surgery in Ethiopia with our Clean Cut program.

