Skin preparation
Appropriate skin preparation of both surgeon’s hands and patient’s surgical site
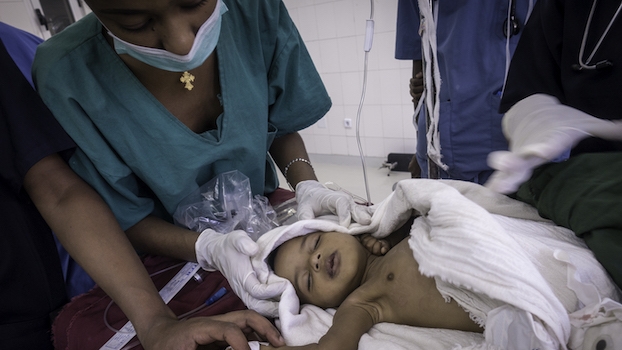
Clean Cut reduces deaths and complications from infections after surgery.
Surgical site infections are a common and devastating complication of surgery. In low- and middle-income countries, surgical patients are twice as likely to suffer from an infection than patients undergoing surgery in the United States.¹
Clean Cut®- the Lifebox surgical infection reduction program – reduces surgical infection by strengthening adherence to six key infection prevention practices. A surgical site infection (SSI) is an infection that occurs in the part of the body where surgery took place and can lead to serious complications and death.
Clean Cut has demonstrated a 35% infection reduction in all surgical patients – with results published in the British Journal of Surgery.² Data showing the lasting impact of Clean Cut were published in The Journal of the American Medical Association (JAMA) Surgery with hospitals maintaining improvements in compliance with all six program infection prevention standards – demonstrating the program’s impact and sustainability.³
Most importantly, for scalability across low- and middle-income countries, Clean Cut requires no major investments in new infrastructure or resources.
Lifebox is scaling Clean Cut across multiple sites and contexts, implementing the program in Bolivia, Côte d’Ivoire, Ethiopia, India, Liberia, Malawi, and Madagascar, and adapting the program to improve the safety of cesarean sections, cleft surgeries, and long bone fracture.
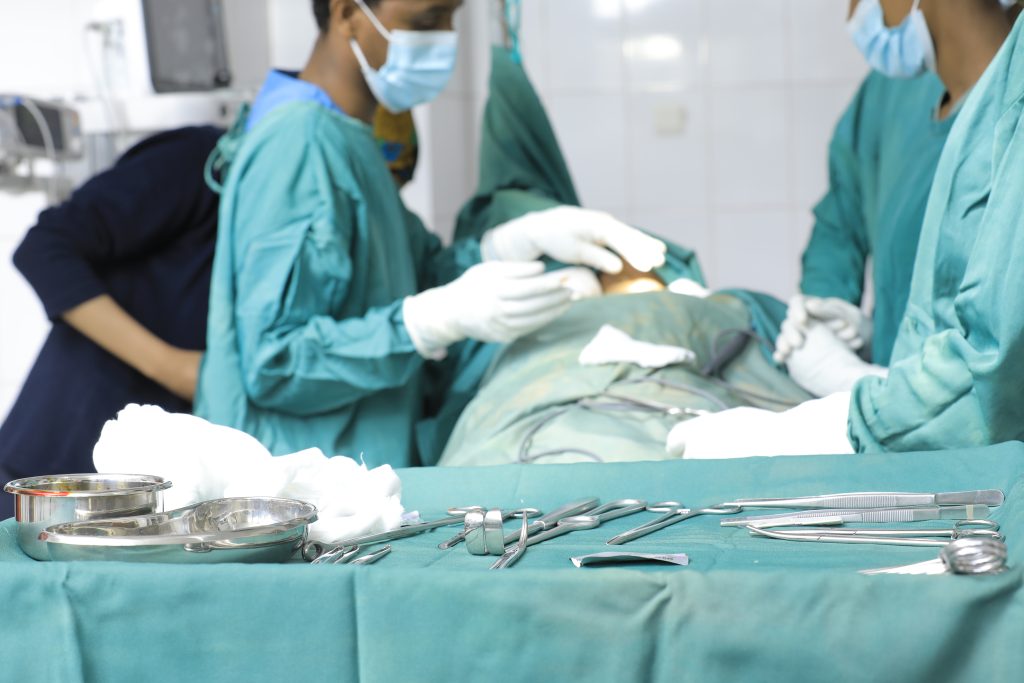
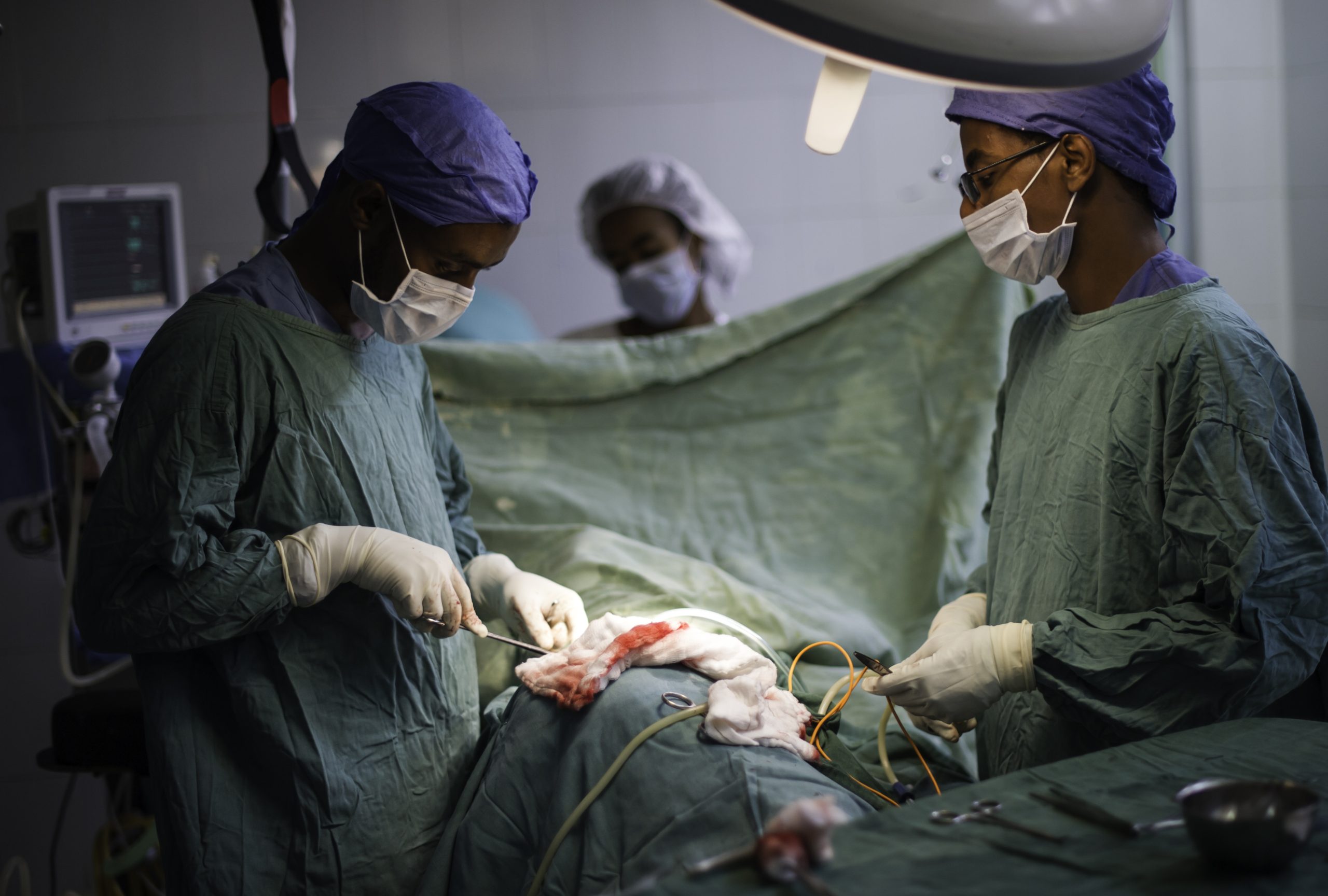
©Lifebox/Yosef Amare Tsehayu, surgical team working at Yekatit 12 Hospital Medical College, Ethiopia.
Appropriate skin preparation of both surgeon’s hands and patient’s surgical site
Administering antibiotics within one hour of surgical incision
Maintenance of the sterile field, including reusable gowns and drapes being washed and sterilized
Covering decontamination, reprocessing, sterilizing, and confirmation of instrument sterility
Counting gauzes at appropriate points during surgery
Effective use of the Checklist to promote teamwork, communication, and a culture of safety
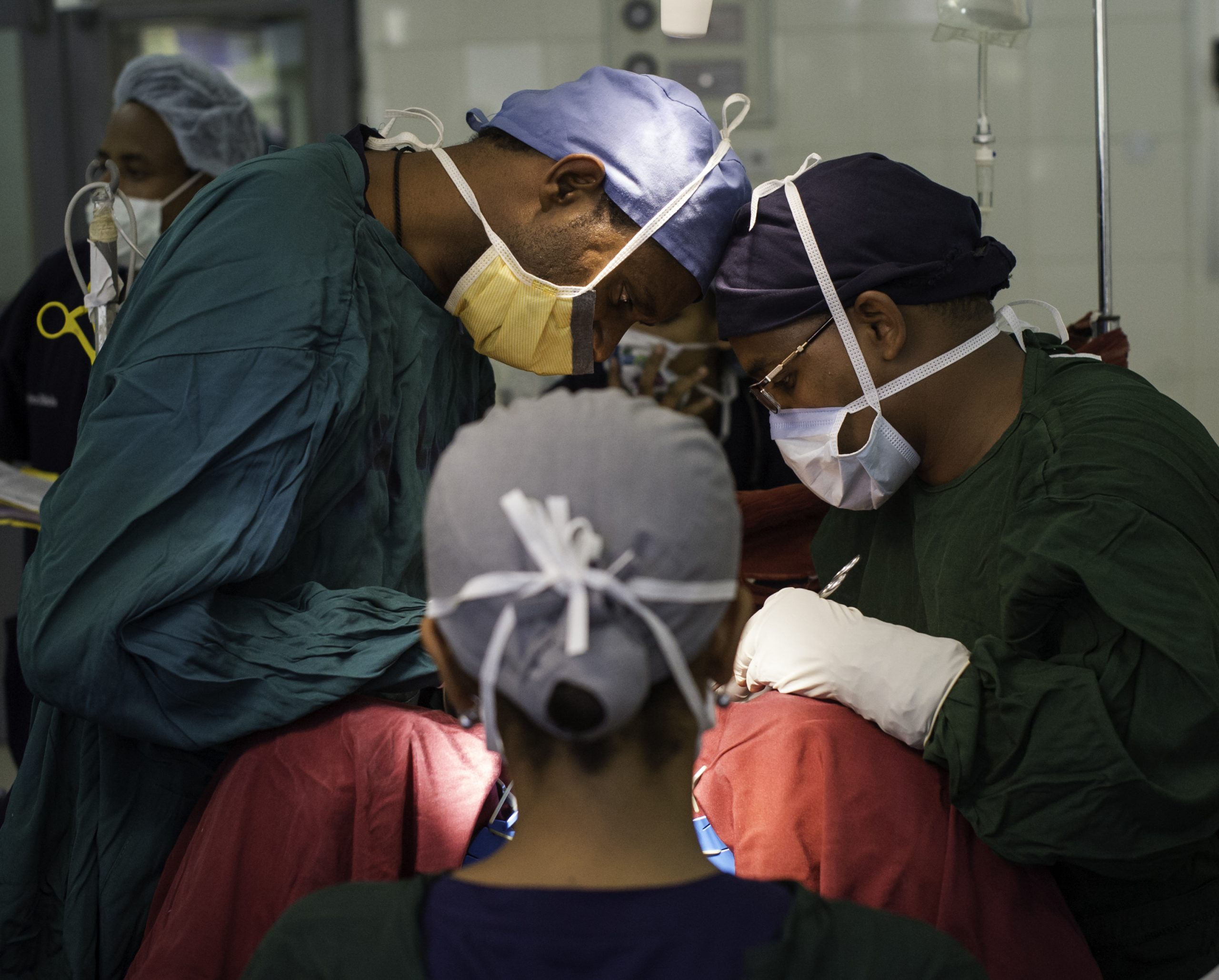
Adapting Clean Cut to improve the safety of C-sections

Tackling surgical infection in Liberia
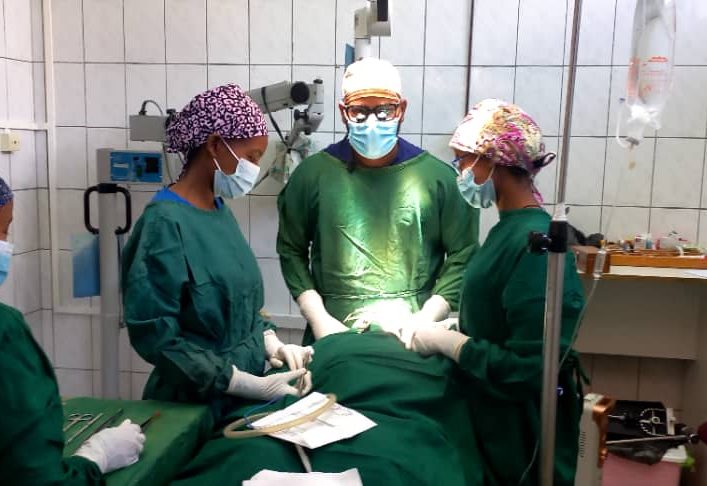
Making cleft surgeries safer
Clean Cut was originally piloted in Ethiopia in partnership with the Ethiopian Surgical Society and the Ethiopian Federal Ministry of Health, with support from the GE Foundation’s Safe Surgery 2020 initiative.
¹ Allegranzi B, Bagheri Nejad S, Combescure C, Graafmans W, Attar H, Donaldson L, et al. Burden of endemic health-care-associated infection in developing countries: systematic review and meta-analysis. Lancet Lond Engl. 2011 Jan 15;377(9761):228–41.
² Forrester J, Starr N, Negussie , T et al. Clean Cut (adaptive, multimodal surgical infection prevention programme) for low-resource settings: a prospective quality improvement study. British Journal of Surgery. 2020 https://doi.org/10.1002/bjs.11997
² Starr N, Nofal MR, Gebeyehu N, et al. Sustainability of a Surgical Quality Improvement Program at Hospitals in Ethiopia. JAMA Surg. 2022;157(1):68–70. doi:10.1001/jamasurg.2021.5569