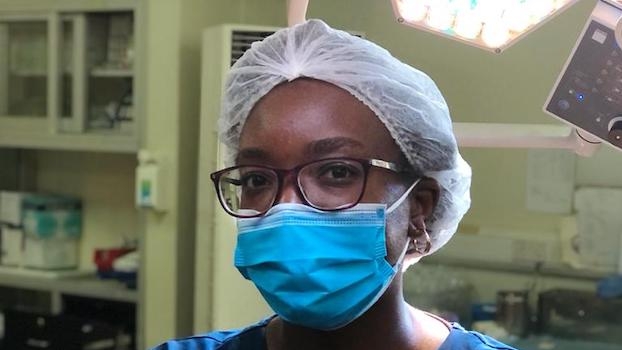
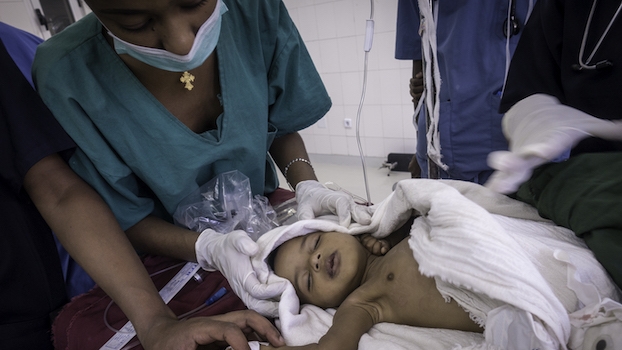
Resources
Find Lifebox resources for perioperative professionals - including publications, our online learning courses, and Lifebox workshop materials
Featured

Online Smile Train-Lifebox Capnography Course
A free online course on the fundamentals of capnography

Scalability and Sustainability of a Surgical Infection Prevention Program in Low-Income Environments
Clean Cut results, published in JAMA Surgery, achieve a 34% relative risk reduction of surgical site infection

Clean Cut (adaptive, multimodal surgical infection prevention program) for low-resource settings: a prospective quality improvement study
This study showed that Lifebox's Clean Cut program improved infection prevention standards to reduce SSI without infrastructure expenses or resource investments.

Operating room efficiency in a low resource setting: a pilot study from a large tertiary referral center in Ethiopia
This study found a high cancellation rate, most attributable to late start times leading to delays for the remainder of cases, and lack of preoperative patient preparation.

Perioperative Provider Safety in Low- and Middle-income Countries During the COVID-19 Pandemic A Call for Renewed Investments in Resources and Training
The ongoing, severe shortage of protective equipment and training gaps should be immediately remediated to prevent the loss of healthcare workers in lower-income environments.
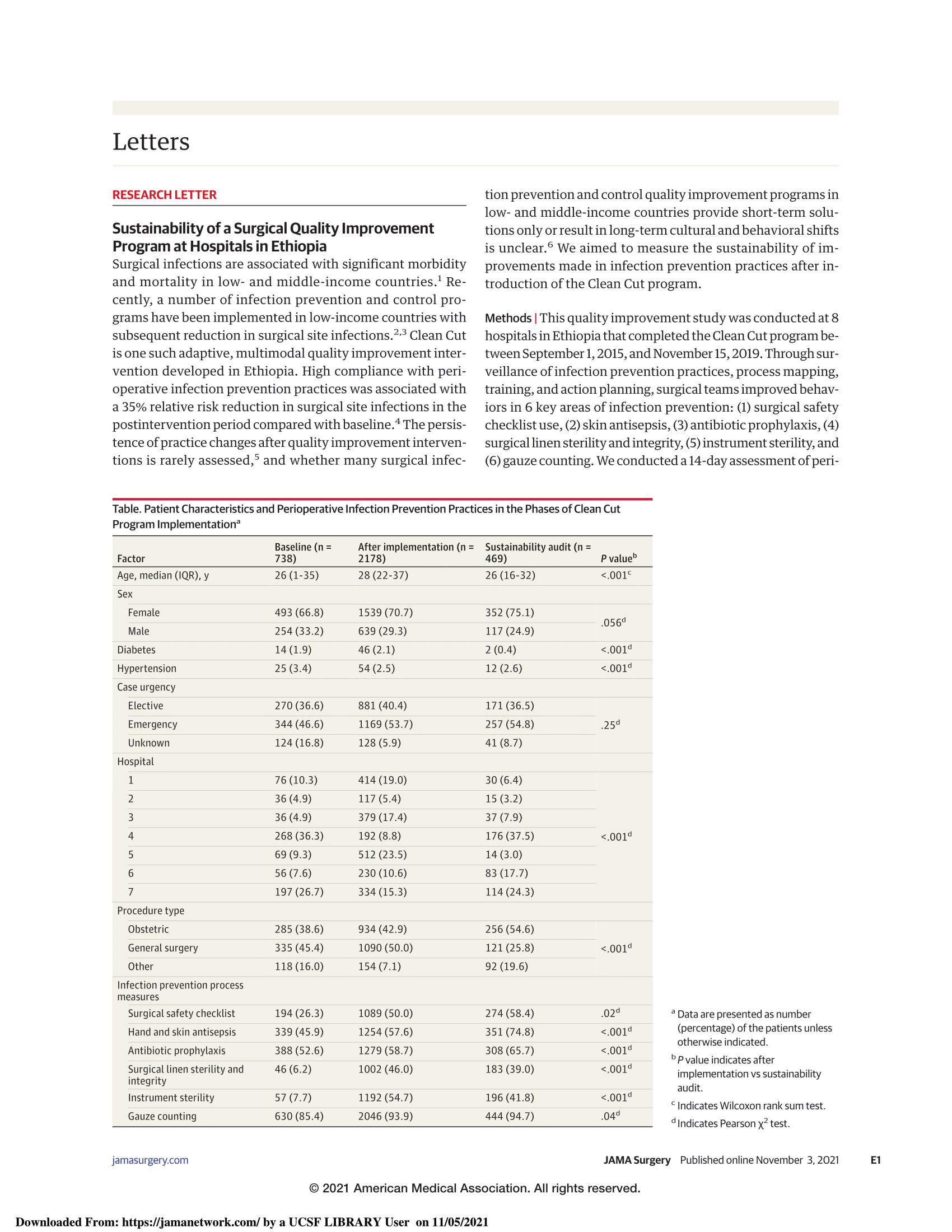
Sustainability of a Surgical Quality Improvement Program at Hospitals in Ethiopia
The results of the lasting impact of Lifebox’s surgical infection reduction program - Clean Cut - in The Journal of the American Medical Association (JAMA) Surgery.

Takuo Aoyagi, Ph.D., American Society of Anesthesiologists Honorary Member
American Society of Anesthesiologists (ASA) awards posthumous Honorary Membership to Aoyagi to recognize his gift to medicine that has literally touched the lives of billions.

Tribute to Dr. Takuo Aoyagi, inventor of pulse oximetry
Dr. Aoyagi’s final wish was to find a theory of pulse oximetry. We hope this tribute to him and his invention will inspire a new generation of scientists, clinicians, and related organizations to secure the foundation of the theory.

Addressing quality in surgical services in sub-Saharan Africa: hospital context and data standardization matter
Like politics, all quality improvement is local, so a deep understanding of local context and circumstances is essential.

Anesthesia facility evaluation: a Whatsapp survey of hospitals in Burundi
This study has demonstrated the feasibility of using a WhatsApp chat group among a national society of anesthesia providers in Burundi to perform an initial abbreviated audit of anesthesia facilities.


Pulse oximetry in low-resource settings during the COVID-19 pandemic
Large gaps remain in other critical units of the hospital, including PACUs, ICUs, and emergency rooms, where on average there were 1–3 unmonitored high-acuity beds per unit.

The Lifebox Surgical Headlight Project: engineering, testing, and field assessment in a resource-constrained setting
No device satisfied all the predetermined specifications, and large price discrepancies were critical factors leading surgeons’ choices.