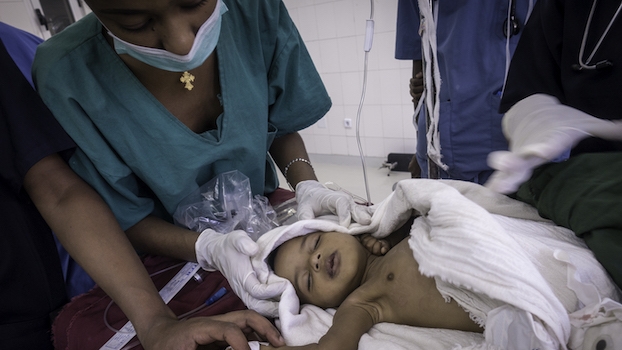
Global Scaling of a Surgical Infection Prevention Program to 5 Low-Resource Countries
A groundbreaking study in JAMA Surgery highlights the powerful impact of Clean Cut, a Lifebox program advancing safer surgery worldwide.
Find Lifebox resources for perioperative professionals - including publications, our online learning courses, and Lifebox workshop materials

A groundbreaking study in JAMA Surgery highlights the powerful impact of Clean Cut, a Lifebox program advancing safer surgery worldwide.

A free online course on the fundamentals of capnography

Clean Cut results, published in JAMA Surgery, achieve a 34% relative risk reduction of surgical site infection

This study showed that Lifebox's Clean Cut program improved infection prevention standards to reduce SSI without infrastructure expenses or resource investments.

No device satisfied all the predetermined specifications, and large price discrepancies were critical factors leading surgeons’ choices.

This study demonstrated that communication is critical, and an effective communication plan within and between facilities, as well as between providers across the health system and even between countries, is essential and should be established immediately.

This Lifebox and Ariadne Labs study - published in the British Journal of Surgery - showed that, worldwide, Surgical Safety Checklist (SSC) use is generally high - with an average of 75% of operations conducted with the Checklist - but significant variability exists.

The findings of this study highlight the importance of engaging hospital leadership, providers and staff in quality improvement programs, and understanding their work contexts.

This study found that the novel reusable pediatric Lifebox probe can achieve a quality SpO2 measurement within a pragmatic time range of weight‐appropriate Masimo equivalent probes.

Safe surgery requires reliable, high-quality lighting. In low- and middle-income countries (LMICs), electricity outages are disruptive, dangerous, and ubiquitous.

This study presents the summative usability testing process of our human-centered design (HCD) approach.

This study indicates that large gaps exist between instrument reprocessing practices in low- and middle-income countries (LMICs) and recommended policies/ procedures.

In this study, enumerating the steps involved in surgical infection prevention using a process mapping technique helped identify opportunities for improving adherence and plotting contextually relevant solutions, resulting in superior compliance with antiseptic standards.

This study found that pulse oximetry was generally deemed valuable by health care providers (HCPs) for use as a spot-check device in a range of pediatric low-income clinical settings.