Published Works
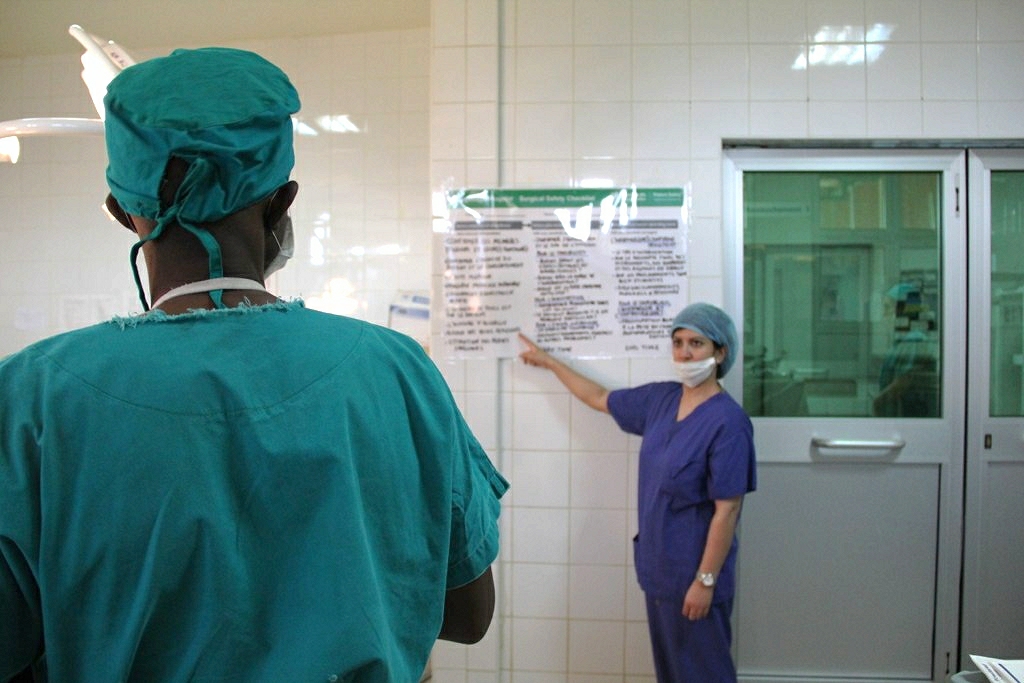
Variation in global uptake of the Surgical Safety Checklist
Delisle M, Pradarelli JC, Panda N, Koritsanszky L, Sonnay Y, Lipsitz S, Pearse R, Harrison EM, Biccard B, Weiser TG, Haynes AB, on behalf of the Surgical Outcomes Study Groups and GlobalSurg Collaborative
British Journal of Surgery, January 5, 2020
https://doi.org/10.1002/bjs.11321
To determine the prevalence and predictors of global use of the WHO Surgical Safety Checklist, this pooled analysis was conducted using five global surgical outcomes datasets (ISOS, SASOS, ASOS, GlobalSurg 1 and GlobalSurg 2), yielding a sample of 85,957 patients from 94 countries. Analyses were presented by country Human Development Index (HDI), a country-level summary measure of development comprised of three dimensions: health, education, and standard of living.
- Globally, use of the Checklist was reported in nearly 80% of patients
- The checklist was used more often in very high (88.8%) and high (87.8%) HDI countries, where middle and low-HDI countries reported Checklist use in 60.4% and 29.8% of operations, respectively
- Checklist use was less likely in emergent operations, and Checklist use decreased down HDI categories in both urgent/emergent and elective operations
- The Checklist was used less often in patients undergoing obstetric and gynaecological surgery, minor versus major operations, and in facilities were the common or official language was not one of the WHO official languages
Since its introduction 10 years ago, the WHO Surgical Safety Checklist has spread across the globe, yet significant variability exists across different resource settings and patient populations.
Forthcoming Publications:
Global Survey of Perceptions of the Surgical Safety Checklist Among Medical Trainees and Early Career Providers
To evaluate the reach of the Surgical Safety Checklist into medical education globally and determine early career providers’ perspectives on the tool, Lifebox and Ariadne Labs collaborated with the International Student Surgical Network (InciSioN ), an international non-profit organization consisting of medical students, residents, and young doctors from all over the world committed to global surgery. The collaborative team performed a survey of 600 members of InciSioN. Representative of the “Checklist Generation,” InciSioN members were introduced to the Checklist after its global introduction. We sought to assess their perceptions of the Checklist and suggestions for its improvement.
A systematic review of the Surgical Safety Checklist in LMIC
To characterize the evidence base of implementation strategies, compliance & adherence measurement, provider perspectives & attitudes, and outcomes associated with the Checklist in low- and middle-income settings, Lifebox and Ariadne conducted a review of all Checklist-related literature from LMIC since 2008. Findings reveal an overall shift from pre/post-Checklist implementation modalities to a focus on promoting checklist use by strengthening the processes embedded within the Checklist, as well as encouraging teamwork and non-technical skill development of surgical teams.