Full report: Checking In On the Checklist
Press Release: English | Spanish | French
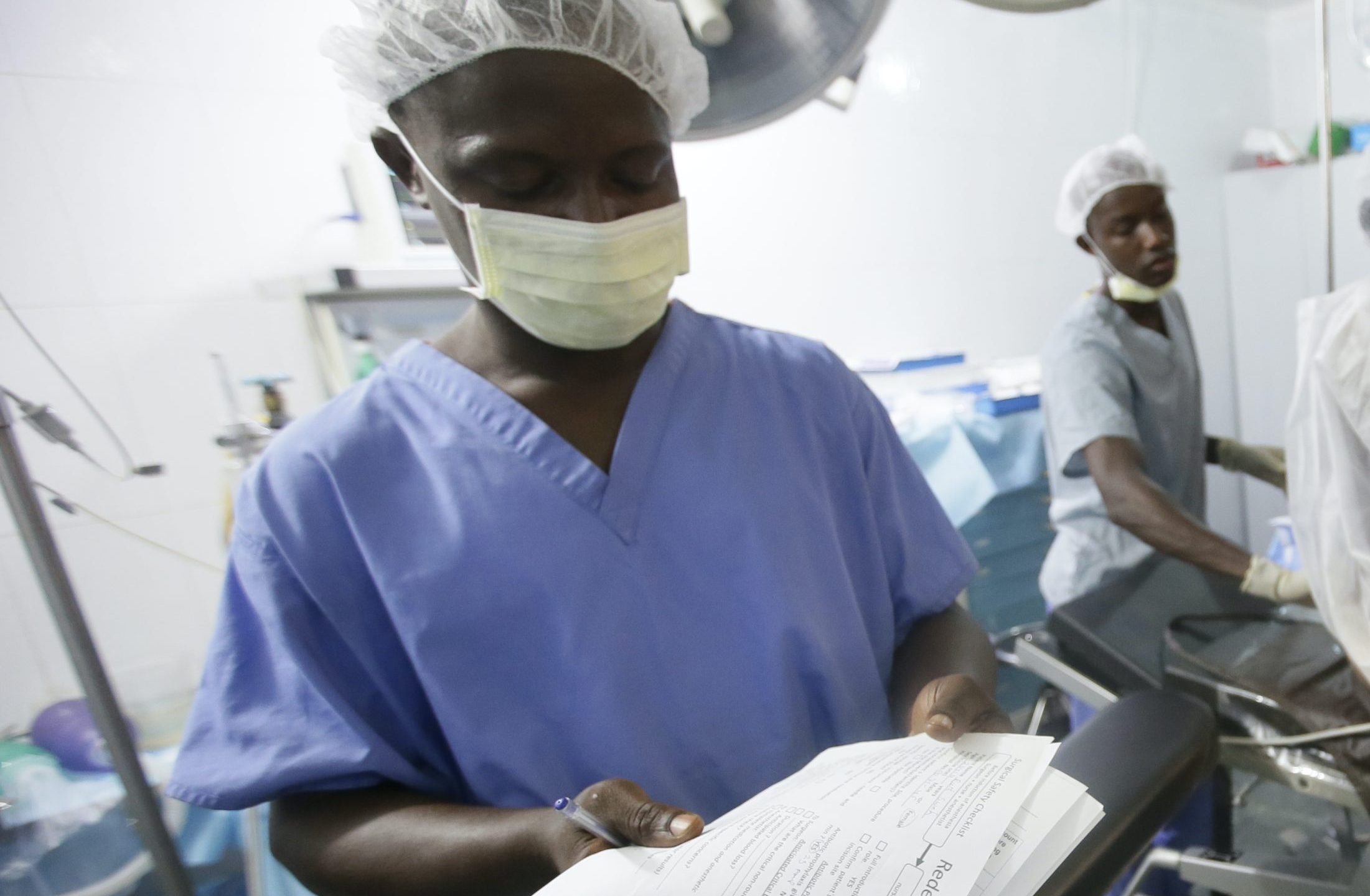
The Checklist—a 19-item list of prompts divided into three critical pause points—was created to prevent “never-events” (mistakes that should never happen in surgery), to promote safe administration of anesthesia, reduce surgical site infections, and improve teamwork and communication in the operating room. A two-year study carried out by researchers from the WHO and Dr. Atul Gawande’s group at the Harvard T.H. Chan School of Public Health examined patient outcomes before and after implementation of the Checklist at eight pilot hospitals in low-, middle-, and high-income countries. The Checklist was found to be associated with nearly 50% reduction in mortality and a 36% reduction in postoperative complications, as well as improved teamwork and communication among members of the surgical team.
A decade after its launch, facilities in 70% of the world’s countries report using the Checklist, and the Checklist is documented as the national standard of health ministries in at least 20 countries, illustrating its widespread reach and appeal. In addition to reducing mortality and morbidity following surgery, the Checklist has had profound qualitative impact, from introducing a culture of safety and improved communication and efficiency in surgical teams, to increasing patient trust and empowering surgical clinicians, and improving job satisfaction.
Despite this impact, this report identifies critical barriers to increased uptake of the Surgical Safety Checklist, especially in low- and middle-income settings, where the Checklist work remains unfinished. Multiple barriers hinder universal adoption: inadequately supported introduction of the Checklist, failure to adapt the Checklist to local contexts, the perception that the Checklist requires too much time to complete, and concerns about impact on existing workflows.
Recommendations
In Checking In On the Checklist, we see that implementation of this seemingly simple tool is anything but a simple exercise. Rather, it’s a complex multidimensional process based on understanding existing power structures and the motivations of those involved, fostering team learning and mutual understanding, and realigning routine practices with incentive structures. The Checklist requires that clinicians embrace a collective mindset, rather than one of individualism and competition.
Key recommendations for successful implementation and sustained use of the Checklist include:
BUY-IN
- Engagement of leadership, including local site leadership and national health officials, to ensure buy-in across all levels
- Engagement of all members of the multidisciplinary surgical team in the implementation process to address potential barriers to the uptake of the Checklist from the beginning
ADAPTATION
- Local adaptation of the Checklist, including modification of its items, language translation, and encouragement of greater participation by all surgical team members
- Tailored implementation of the Checklist based on local context by including all stakeholders in the implementation design and improving the implementation process through feedback from frontline implementers
ACCOUNTABILITY AND SUPPORT
- Building accountability structures by balancing top-down with bottom-up approaches to Checklist implementation, depending on the context
The WHO Surgical Safety Checklist is more than a single sheet of paper with 19 items. It is a vehicle that promotes patient safety, teamwork, effective communication, and empowerment of operating room staff who have traditionally been voiceless. These past ten years have demonstrated that effective implementation of the Checklist can lead to extraordinary improvements in patient outcomes following surgery. We have also learned that implementation of the Checklist can be difficult, and that the impact it stands to bring to the operating room depends on the quality of how the Checklist is implemented and reinforced. We have ample evidence that the WHO Surgical Safety Checklist works. The next challenge before us is how to promote and effectively implement this revolutionary tool throughout the world, especially in low- and middle-income settings.
Checking In On the Checklist is a report by and for people who use the Surgical Safety Checklist around the world, and those who are interested in learning from their experiences. We hope that it serves as a roadmap for the role of the Checklist in global surgical safety over the decade to come.